Community and collaboration are central to our approach to care technology and Nourish. We depend upon the insight and experience of our users to shape our future. That is at the core of a true digital partnership in social care, co-production. At this year’s Nourish Customer Conference, hosted in the gorgeous Goodwood House, we came together with care professionals, partners and the wider Nourish community for a day centred around collaboration, innovation and shared purpose.
Our recap video captures the atmosphere, ambition and energy of the event. Highlighting the insightful presentations and product discussions. As well as the moments of connection that happen in between sessions.
The conference was an opportunity to reflect on how technology, partnership and co-production continue to shape the future of social care. Throughout the day, attendees explored new ideas, shared experiences from across the sector and discussed the challenges and opportunities facing care providers today.
One of the strongest themes throughout the Goodwood House Nourish Customer Conference was the importance of working together.

The day showcased the collaborative spirit that continues to drive the development of the Nourish digital ecosystem. From product roadmap discussions to shared experiences from care organisations across the UK. The day reinforced the value of listening, learning and building together.
This commitment to co-production remains central to how we approach innovation at Nourish. We work with providers to ensure that the technology we create is shaped by the real experiences of the people delivering and utilising care every day.
Attendees explored emerging developments across the Nourish platform, including data, AI, transparency and safety. In addition to broader discussions around the future of care technology and operational sustainability.
As with previous Nourish events, the focus was not simply on showcasing technology, but on understanding how digital tools can support better outcomes, stronger communities and more person-centred care.

The energy of the Nourish Customer Conference was electric. It reflected the optimism and momentum shared by everyone who attended.
Social care continues to face significant challenges. But events like the Goodwood House Nourish Customer Conference remind us of the innovation, compassion and expertise that exists across the sector. By bringing together people with shared values and a shared ambition to improve lives, we can continue building technology and support systems that genuinely make a difference.
A huge thank you to everyone who joined us at Goodwood House and helped make the day such a success. We’re excited for what comes next and look forward to continuing the conversation together.
We all understand the importance of valuing and respecting those we care for, when we speak about how you can truly deliver dignity in care, it might be hard to conjure up an exact idea of what that really means or looks like. Luckily Dignity in Care has come up with the 10 Dignity Do’s. An easy list that describes the values and actions of a high-quality care service that respects and upholds people’s dignity to the highest standard.
1. Have a zero tolerance of all forms of abuse
2. Support people with the same respect you would want for yourself or a member of your family
3. Treat each person as an individual by offering a personalised service
4. Enable people to maintain the maximum possible level of independence, choice and control
5. Listen and support people to express their needs and wants
6. Respect people’s right to privacy
7. Ensure people feel able to complain without fear of retribution
8. Engage with family members and carers as care partners
9. Assist people to maintain confidence and positive self-esteem
10. Act to alleviate people’s loneliness and isolation
A Dignity Champion is a person who believes that being treated with dignity is a basic human right, not an optional extra. They believe that care provision must be: compassionate, person-centred, efficient and effective, and are willing to take action in order to achieve this.



Dignity Champions are those in a care organisation that champion and uphold the 10 Dignity Do’s, as well as advocate and share the importance of dignity in any form of care. This includes:
1) Standing up and challenging disrespectful behaviour
2) Acting as role models by treating other people with respect, particularly those who are more vulnerable
3) Raising issues regarding dignity to improve the way that services are organised and delivered
4) Influencing and informing colleagues on best practice
5) Listening to and understanding the views and experiences of those in care
You can find out more about becoming a dignity champion and the 10 Dignity Do’s by visiting Dignity in Care’s becoming a champion or register page. Another helpful resource is the Dignity Champion’s Toolkit for Action, which includes actionable insights, ideas and advice for people in a range of different care roles to help make a difference and bring dignity to care.
There are many ways that the Dignity Do’s can help care groups, teams and organisations improve their level of care and adapt to offer a continuously improving level of service. Championing the Dignity Do’s is only the start, we believe that in order to provide the highest quality care, moving to digital care planning enables you to create personalised care plans, record care accurately at the time of providing care and understand and act on trends about those you care for. By using digital, you can be much more efficient and spend more time providing person-centred, quality care.
To find out how care software and technology can be used to enhance your care service, or help you to better care for those you support, book a demo with the team.
Anthropic recently published a new constitution for ‘Claude’, their Gen AI model. The AI is designed for natural conversation, complex reasoning, coding, analysis, and content creation. Anthropic was founded with the aim of creating AI with a focus on safety and ethics. An ambition shared in the health and care sectors, where safety is a paramount concern given the huge responsibility communities entrust in their care and support providers. Throughout their technology’s iterations Anthropic repeatedly look to connect their functionality to human values. This approach resonates with us at Nourish, where we firmly root our AI models in lived experience by always keeping a ‘human in the loop’ throughout the design process. We believe principals are essential for applied AI, as we continue to search for the most impactful and effective applications of AI in health and care technology.
Our director of Data and AI, Sudha Regmi, saw several parallels between Claude’s new constitution. Here are her three key takeaways from the recent announcement.



“When you’re raising kids, you can’t just hand them a list of rules and hope it covers every weird eventuality life throws at them,” explained Sudha. “You try to teach values and principles, then trust they’ll generalise when it matters.”
Anthropic is basically saying the same thing. No, not that all GenAI is inherently attention seeking and impulse driven. (That’s just a good portion of the user base). They are saying, don’t just tell the model what to do, teach it why with context. This gives the model the ability to generalise across novel situations. With ‘rules’ in place, GenAI can become confused by edge cases. With ‘principals’ the model is better designed to understand context and infer the correct decision.
“This is an understandable but misleading hangover from early AI scepticism. Pretraining is very important for AI models, but is not the be all and end all, especially for applied AI. Post-training is also very important. Along with feedback loops, policy layers and product choices. When choosing how to apply AI models to modern challenges, there is no predictable answer. We must, to borrow a technique from social care, review our impact, continuously improve and remain connected to lived experience.”
No two experiences are exactly the same. You can see this in the real world with “the same base model” behaving differently depending on where you use it. Put the same prompt into different models and look at the output. These differences express themselves across both different models and different iterations. For example, think about the difference in output when you have Copilot (in gpt5 mode), ChatGPT or OpenAI GPT models doing the same tasks via APIs. Or the differences when using Claude Sonnet in Claude Code vs Claude Cursor.

There are vast differences in models that share similar origin stories. Applied AI will continue to develop in a huge variety of fields. We must be able to more deeply understand the context of the model, before we can effectively teach the model the context of its application.
“The constitution is explicit about priority order: safe → ethical → compliant → helpful. It includes ‘hard constraints’ for especially high-stakes work. It validates that the process of building AI is just as important as the product.”
The process of building applied AI is crucial. Principles are deliberate, and they can’t just live on a slide deck. They must be represented in your approach to AI design, including:
Incentivising the right kind of outputs for the context
Health and care are not vibes-based domains. Decision carry a huge amount of weight and privacy. Context is essential for understanding both best practice and the reality of the responsibility.
Human-in-the-loop validation with clinical experts
Lived experience remains the alpha and the omega for technology design. Without human input into the design process, AI can never be considered responsibly designed.
Tight feedback loops with our customers to pressure-test what “good” looks like in practice
That’s what breeds confidence in applied AI. Not reverential ‘this is what the model said to do’. Not black box decision makers. But results driven by a combination of principles, process and validation.
If you’re building with AI right now or even thinking about adopting AI tools, we’d recommend reading the constitution. Even if you disagree with parts of it. It’s a useful window into how one lab is translating “alignment” into something operational.
If you want to know more about Nourish Care’s approach to applied AI for health, care and support, click here.
Social care is in a state of change. Care providers tasked with being the steady hand through this change have consistently risen to the challenge. Despite having little control over the changes as they happen. At Nourish Care we are embracing this change by working with our users to develop a social care future we are all proud of. With increasing standards, new regulations and extended funding availability it is clear now why so many care providers are embracing change themselves and switching to Nourish.
Care providers have a wealth of options when choosing a digital partner. Under the original standards for the NHS Assured Solutions List (ASL) there are 24 Digital Social Care Records (DSCRs) to choose from. That’s without mentioning the systems who don’t reach these standards. The ASL is enjoying notable success so far, as it continues to work towards its target of 80% of care providers on DSCRs. Digitisation is widespread through social care now. To the point that many care providers are shopping around for a better system to match their service.
The ASL was always intended as a starting point for the digitisation of social care. The Department of Health and Social Care has announced the second step of this journey, with the recent release of the 14 new standards for DSCRs on the ASL. We are one of the few providers to have achieved all 14 of these standards. You can read about the specifics of the standards here.
We are the largest software supplier to have achieved the new standards. As well as being one of the first to get listed on the ASL following its initial launch. Our legacy of forward thinking and innovation consistently aligns us with the future direction of the social care sector. We are proud to be working closely with key decision makers in health and social care.
We support care in a huge variety of settings. Including older person’s care, nursing, home care, learning disabilities, dementia, supported living, assisted living, substance abuse, mental health, children and young people and more. Each care setting is unique, and each care setting requires specific understanding to support effectively.
Our experienced and understanding customer success and support teams will work with you to make sure our system fits your service. Whatever your needs are, and whatever they may become in the future.
Once you switch to Nourish, we are with you every step of your journey. Should your journey lead you to new business opportunities we are the best equipped software supplier in social care to support your expansion. Whether you are focussed on a single type of care or support a range of different needs.
You can also scale your functionality as desired, thanks to our comprehensive partnership programme. The programme unites key best-in-class innovators like Camascope for eMAR, Radar for incident management and PainChek for pain management. All while keeping a finger on the pulse for emerging technologies that will substantially impact the social care sector.
Additionally, we offer more in-depth data packages called ‘Insights’ and ‘Analytics’. These features provide a much richer insight into the data gathered across your service. Perfect for larger care providers who collect vast swathes of information every day, but have no clear way to transform this potential into insightful, actionable information.
The Care Quality Commission’s (CQC) rollout of their new Single Assessment Framework (SAF) is enduring some understandable teething challenges. Initialisms aside the ambition of the project remains clear. The regulator wants to streamline processes and better respond to the needs of the people who draw upon care.
We facilitate these new developments as effectively as possible. We work with organisations like the Care Software Providers Association (CASPA) to share our voice and insights on the development of digital social care with key decision makers in local and national government. Our work on alignment with #socialcarefuture helps to guide the future of our system as much as they guide the future of the wider care communities. Socialcarefuture are the co-authors of the ‘I/We Statements’ that define the SAF scoring.
There is always something new to be considered, a fresh function to be explored or a new piece of legislation to be adhered to.
We cannot know the future; all we can do is prepare for it. We have read the tea leaves, built our houses from stone and made hay while the sun shone. All so we can continue to lead the way in digital social care, through innovation, understanding and collaboration.
Social Care is in a state of change, and with that ever-present uncertainty comes a great opportunity. Switch to Nourish today and take control of your change, with your team, your service and your community.
A digital ecosystem is a community, where everything is interconnected.
They come in many sizes, shapes and circumstances. Each one supporting life in a unique dance of differing dimensions. As technology continues to develop in health, care and support these dimensions are becoming increasingly distant. Many technology suppliers are simply recreating the physical silos of information in cyberspace. We can’t replace filling cabinets with isolated servers and expect to move forward, we certainly can’t do it and expect to improve the quality of support people receive! At Nourish we want to build ecosystems, not just platforms. Ecosystems shaped by interconnectivity across systems, and data sharing that is both straightforward and secure. That way we can ensure that providers have access to all the information they need, care and support professionals have the tools to deliver outstanding standards and crucially, everything is centred around the person utilising the service.
From the very beginning, Nourish has been built on one simple but powerful belief: the person supported matters most. This belief is why we develop all our functionality through coproduction. Our commitment to collaboration throughout our platforms. Thanks to this approach every year our understanding of care is deeper, our experiences wider and our expertise sharper than the one before. Because we operate as a true digital partner, we continue to grow with our users throughout their journey.
The past few years have shown us the potential for technology in social care, while Nourish users have revealed to us the best applications for our software, opening our eyes to the opportunities for supporting positive change in the wider system of care. In response, we consistently and continuously update our existing functionality, and look for spaces in the needs of our users to develop new platforms.
This expansion of our application is rooted in keeping people at the centre of our systems. We know growth demands structure, scaling demands clarity, and crucially, care demands trust. Structure can be built, clarity provided but trust, trust must be earned.
Nourish Care impacts 1 million people every day. A responsibility we are both very proud of and deeply committed to.
We know no two people with support are the same. Uniqueness is the blessing, and the curse of social care. One size will very much not fit all. You need the right tools for the job, and the best people behind them to support you.
We designed our ecosystem to start at the beginning, with the person supported. From there you can build out your functionality to fit your service, wrapping the right systems around the unique shape of your community and their needs. A successful ecosystem gives you the freedom to grow as you want, and the stability to maintain what you need.
We can’t predict the future (yet) but with the right tools we can always prepare for it.
Nourish Better Care is our system built for residential settings. Designed to be easy to use for carers, and straightforward to review for care managers, it comes equipped with the tools you need to capture the full picture of every life you support.
Nourish Safety gives you a holistic, detailed tool. To manage incidents, ensure compliance, and focus on what matters most, driving lasting improvements in care quality.
Nourish Confidence is a single place to unify audits, actions and AI‑assessed care plans to support better decision‑making across your service.
Nourish Transparency is a new way to bring clarity to your care planning and help you understand the true cost of your care. Enabling providers to take a more structured, data-informed approach to planning and resourcing care and support.
Nourish Insights helps care providers manage, review and understand their data with our easy to read and action dashboards.
Nourish Empower offers industry leading rostering functionality. With an easy-to-use app, workforce management and accurate call monitoring giving home care providers everything you need to support your community.
Nourish Better Care at Home builds upon this base with more detailed point of care functionality. To support truly mobile first care by offering richer interactions, contextualised care plans, in app messaging and robust point of care functionality.
Nourish eLearning is our inbuilt partnership with MyAko. A Skills for Care and CPD accredited eLearning provider, to deliver an all-in-one digital learning solution for home care agencies.
Nourish Protect enables your team to efficiently record and access information at the point of care, whilst ensuring sensitive data remains secure and protected.
To make it easier to find the right products for your community we created this overview of the Nourish Product Ecosystem. Each circle reflects a different focus for our products and the impact it will have on your community.
Care Delivery – For Feeling Supported
Technology that steps back, so care can step forward.
Continuous Improvement – For Feeling Assured
Because confident carers create safer, more consistent outcomes.
Operations – For Feeling Secure
Supporting care teams to be prepared, skilled, and sure of what comes next.
Connectivity – For Feeling Connected
Bringing together every piece of the care puzzle around the person.
This approach goes beyond categorisation. It lays the foundation from which every new product, every innovation, and every solution we launch builds towards something bigger. Including the developments with our partners in the Nourish Partnership Programme. All feeding into a digital ecosystem that fits around your service, and elevates your community.
Most importantly, it ensures that as we scale, we never lose sight of what made us great. Keeping the person supported at the centre of care.
Imagine a health and social care system where care teams feel empowered instead of overwhelmed. Where families feel reassured instead of disconnected. Where people receiving care feel safe, valued, and heard.
That’s the world we’re building.
And we’re not waiting.
We have coordinated internally.
So our teams live and breathe this philosophy.
We are communicating externally.
So our customers feel the impact as soon as possible.
We will continue to co-produce.
Because technology should evolve with the people it serves.
Connections are the core of community. Whether online or out in the world, it is our ties that bind us, and our relationships that lift us up. At Nourish we know the best results come from working together. We want to build partnerships, coproduce platforms and create a digital ecosystem that informs, invigorates and elevates everyone it impacts, every day.
We’ve got lots of exciting plans coming soon, if you want to build the future of social care with Nourish, contact us directly today.

Communication defines relationships. Whether personal or professional, the success of our relationships rests on our ability to communicate effectively with one another. In care this is understood clearly. Care providers go to incredible lengths to better understand, empathise and involve the people utilising support in their service. The same approach can be applied to your relationship with the regulator of your social care compliance. Regardless of the regulator of your service, talking to people to better understand the care you provide will be a central part of their inspection process. Preparing the people in your organisation for these conversations is crucial to taking control of your compliance rating. We explore how you can work on your team’s ability to communicate clearly with your regulator in this blog. Starting with your care and support team, before moving to managers and leaders, and finally central operations and quality assurance. Each of these conversations will vary in approach and focus but are unified by their ability to impact your inspection rating.
Your care and support teams are your direct connection to your community. They interact every day with the people drawing upon your support. This gives them an intimate knowledge of the needs of your community, the processes and philosophy of your service as it is applied in action. A role that requires them to be excellent communicators. So how can you best help carers prepare for a conversation with an inspector?
Confidence is king.
Confidence in the care they provided, confidence in the information recorded, confidence in their approach and pride in the results. Inspectors want to see the care you provide, but they also want to ensure your carers know how and why they are providing it. Carers with a more formative role in the care development will naturally be more confident when describing it. Building this confidence over time for other carers is a matter of engaging with your team. Ask practice questions to help them familiarise themselves with the process and become more comfortable.
Confidence with their care management system is also crucial. The right system is an accessible resource for carers to evidence their care and demonstrate their understanding. This is especially true for agency staff. Accessible records offer a level of familiarity with your service that agency staff can draw upon. Creating a continuity of care that underpins quality social care compliance.
It’s important to remember the inspector’s perspective. Your rating is more than the evidence you provide; it is also dependent on the inspector’s ability to comprehend it. A clear and easily navigable software system can help make this information simple to access and follow for inspectors. You can offer them their own login to explore. Or have a carer guide them through the system, highlighting the work they do, their understanding and efficiency. This rings especially true for agency staff. Agency staff using accessible care management systems find it easier to fit into the unique structure of your service.



A care management system offers you the ability to record your care accurately. This data is central to your social care compliance. When managers can draw specific and detailed reports they can take more confidence in their conversations. Not just in demonstrating the service they provided, but, crucially, pointing to the outcomes of your care.
Ownership breeds confidence, just ask anyone with a BMW. When your care managers and leaders feel like the owners and drivers of the care they provide, they will be in the best position to talk about its quality. Pride might be a sin, but it is deadly effective in inspection interviews. When the work you do helps people live their best lives it is natural to take pride in it. Anything else would be unfaithful to the spirit of care. Managers that can harness this pride, and evidence improved outcomes over time, are well positioned for any inspection.
For central operations and quality assurance team members you want to be able to show the big picture. This means being able to communicate your approach to oversight and how feedback cycles through your service in a responsive manner. Showing your processes backs up the evidence provided on a more specific level by your carers and managers. Reinforcing the quality of your care.
Social care compliance is linked to your policies and procedures. You need to be able to present them and demonstrate how you implement them. Again, this comes back to confidence and ownership as outlined earlier. Care management software can also support you. Simplifying the recording, reviewing and reporting of your policies and procedures.
Additionally, quality care management systems include an ‘audit trail’. This records every change that occurs on your system. Each assessment, each care plan update and all the clicks in between. This gives you a clearly evidencable history of activity on your platform. Painting a picture in real time of the journey of your care, the reality of your policies and the effort of your team.
Relationships are hard, ask anyone whose partner owns a BMW. Communication is the bridge that we build between each other. And whether you are building a bridge between people utilising your service or the people inspecting it, its strength will be defined by the clarity of your communication. This is true to the point that being able to demonstrate the effectiveness of your approach to internal communication in your service is an indicator of quality care.
But, and it’s a big but, effective communication is not telling people what they want to hear. It is telling them what they need to know. This includes pushing back when you feel misrepresented. You are the expert in your service. Set a standard of open, clear communication with your inspector and you will have the confidence to speak the truth to power. Clarity is rarely achieved easily. With confidence in your service, and the evidence to prove your points, clarity is the result that will earn you the rating you deserve.
The biggest show of the social care calendar is right around the corner, Care Show Birmingham. The biggest show attracts the biggest names for the most important conversations. This year we are sponsoring the Care Keynote Stage and we are so excited!
There is a wealth of experience and insight on display on the Keynote Stage in Birmingham. Day 1 is loaded with leaders, lessons and laughs. We contacted the speakers taking to the Keynote Stage for some sneak previews of what they will cover. From state regulators to self-regulation there are several great talks, and only one place to see them.
While you’re visiting the show make sure to come say hi to us on stand G40!
Here’s our Nourish insight into the speakers on the Keynote Stage on Day 1, Wednesday 9th October.



10:30 – 11:00
Speakers
Mark Topps, Co-Founder and Director, The Caring View
Adam Purnell, Co-Founder and Director, The Caring View
Caroline Barker, Legal Director, Healthcare Regulatory
Julie Garrity, Independent Health and Social Care Advisor
The Caring View is a well-known and highly regarded source of useful information and important conversations in social care. Join the hosts, Mark Topps and Adam Purnell as they welcome Caroline Barker, Julie Garrity and the entire care community to a cool-headed conversation on one of the hottest topics in our humble sector, regulation.
“The focus of our conversation with be, ‘how can we ensure compliance with the regulator with regards to care quality?’ So, we’ve got Julie Garrity, who’s an ex CQC inspector and social care advisor, and Caroline Barker from HCR law joining us. We’re going to talk around. Obviously, we know that there’s loads of confusion out there around the single assessment framework. Plus we’re all waiting for Dr Penny Dash’s full report into the CQC. HCR law has seen an increase in people contesting the outcome of their reports. Julie and other consultants have said they’re inundated with providers that need support. Our goal is to triangulate everything that’s going on, all these different sources of information and experience, to focus on how providers can actually just look forward, be streamlined, and leave the framework as it is with all the changes that are going on.” Mark Topps, Co-founder and Director – The Caring View
11:05 – 11:35
Speaker
Matthew Stewart, Chief Product Officer, Nourish Care
Our own Chief Product Officer, Matthew Stewart, will be treading the Keynote Stage boards on day 1. With an extensive background that covers a range of sectors, Matthew understands the crucial moment care technology has reached. There are huge opportunities for care providers and digital suppliers to come together and co-produce effective solutions for everyone in care.

“I love a good challenge. Throughout my career the challenges I faced were consistently about transformation. I worked in many different sectors, but always at the same moment, when there is the opportunity for change, for an industry to take the next step and move forward. As Chief Product Officer for Nourish I recognise that same point in social care. Now is the time for us to face the challenge of utilising digital care systems effectively and take the next big step in quality care. It will not be simple, and it will rarely be straightforward, but we already see positive examples emerging across social care. Join me for an open and ambitious conversation covering what we have achieved already, and what more we can achieve together.”
11:50 – 12:20
Speaker
Dr Ant Webb, Founder, Switched on Thinking
Dr. Ant, also known as the Brain Whisperer, empowers people through the art of positive mind practice. In a world of constant stress, pressure and responsibility it is no surprise so many carers are facing burnout. Join Dr Webb for an inspiring keynote on stress management and mindset empowerment, designed specifically for the care sector.
“In this session, I will introduce my powerful Switched on Thinking® methodology, showing how caregivers can shift from reactive to proactive mindsets. I can help carers learn how to identify emotional triggers, manage stress before it escalates, and foster collaboration within their teams to enhance resilience. Through practical tools like the Circle of Awareness®, attendees will leave with actionable strategies to improve their own well-being while enhancing the quality of care they provide. This is a must-attend talk for those looking to build a stronger, more supportive care environment while preventing burnout and enhancing team cohesion. Don’t miss this transformative session!”
13:30 – 14:00
Speaker
Big Ian Donaghy, Chair
The sweet tooth from chocolate city, Big Ian Donaghy will be the Chair for the Keynote Stage. He will also be taking to the stage himself just after lunch to talk about how we can all benefit by supporting neurodiversity in care.
“My talk is about why we need to embrace the neuro divergence population into care. If we want things to stay the same, then we need to be bringing people into care who just think the same and do the same and are happy to do the same. Whereas, if you want to create change, you need somebody who looks at things differently. Someone who does things differently and someone who maybe treats people differently. We need people in care who are different, not worse. People in care who are different, not less. We need people who are magnificently different to create change, to make care better. So, I’m doing a big thing about why we need to go looking for the people who view things differently so that we can revolutionize care.”



14:15 – 14:45
Speakers
Vikki Beckwith, Managing Director, The Affinity Care Group Limited
Tiffany Nelson, Operations Manager, The Affinity Care Group Limited
Regulators are a common source of consternation in care. Inspections are always going to involve stress; it is a natural part of the process. Providers know how important it is to put their best foot forward in these situations, but do you know how? With recent reforms and reports there remains an air of uncertainty when evidencing to the CQC. An air that Affinity Care Group are looking to help providers dispel with their informative and actionable afternoon talk.
“At the Care Show Birmingham this year, we’re covering a topic that I believe many care providers will find valuable. Evidencing for a CQC inspection is a major challenge for many in the sector. As a business, you may be doing everything right, but if you can’t evidence it properly, your rating could be impacted. Last year, we focused on navigating the CQC’s new Single Assessment Framework, but this year, we’re shifting to a more actionable topic. Our hope is that attendees leave with the confidence and knowledge to excel in their next CQC inspection.” Vikki Beckwith, Managing Director – The Affinity Care Group Limited
15:00 – 15:30
Speakers
Angela Boxall, Chief Executive Officer, Majesticare Luxury Care Homes
Diane Danzebrink, Consultant, Speaker, Educator & Author, Menopause Support
Menopause is a big topic, one that has a profound impact on the social care workforce. However, it is too frequently relegated to small conversations. Join Angela Boxall and Diance Danzebrink as they take on the big issues at the heart of menopause and how care providers can improve the support and understanding they offer.
“In our session I will be sharing an overview of the diversity of the menopause experience to help organisations understand how they can offer help and support to colleagues, whatever their menopause experience. My own experience made me acutely aware of just how difficult it can be to navigate the confusing worlds of menopause and mental health without the right help and support. As a result, I combine my professional therapy skills, experience and nurse training in menopause to focus on providing factual, evidence-based information and support to help others navigate menopause and mental health.” Diane Danzebrink – Menopause Support
With so many great options for attendees at Care Show Birmingham 2024 it is understandable to have your attention divided. Make sure you make time for some of the engaging sessions we have listed above. And don’t forget to come visit us on stand G40, we’ve got plenty more surprises in store!

Community is at the heart of quality care. At Nourish Care we are indebted to our community of users, one that spans a range of care types and locations in the UK. We know that the best results come from clear communication and committed collaboration. Our users frequently provide the inspiration and insight that drives the development of our platform. So, it is only natural that we are always looking for opportunities to connect directly with our users. This summer we welcomed over 70 of our valued users to The Gherkin in London for our customer conference. The conference took place over an afternoon and featured idea sharing, our latest product road map and some inspirational talks from guests and Nourish leaders.
The best place to start is always at the beginning, and there’s no better beginning than a drinks reception. The conference kicked off at lunchtime with a selection of drinks and ‘mocktails’ provided by the lovely Gherkin staff. It takes two separate lifts to get to the iconic floor 39, known locally as ‘The Helix’. The magnificent view of London’s skyline slowly started to fill with chatter as the attendees made their way up. The sound of conversation quickly filled the floor and provided a wonderful soundtrack to the view.

Once everyone had proceeded upstairs to ‘The Iris’, the famous glass dome at the top of the Gherkin for lunch, a delectable chicken ballotine followed by a lemon and ginger posset, it was time for the presentations. The first speaker of the afternoon was the incredible Dr Waheed Arian. The doctor, humanitarian, and innovator shared his story with the audience and his perspective on ‘the business of compassion’. Everyone in the room shared his vision of providing health and care support through passion. He detailed the sense of pride and joy we all receive from working with people, and implored attendees not to fall victim to overt self-criticism at our perceived failures. The last question, ‘what does care mean to you?’ carried with it an implicit instruction, ‘Do not lose sight of what you mean to others’.
We all took a break following Dr Arian’s evocative presentation. Upon returning it was time for the Nourish representatives to take to the stage.

First up was Nourish founder Nuno Almeida. Nuno took us through a brief history of the past few years, the pandemic, supply chain issues around the world and reassured us all with the fact that quite frankly, ‘there is no return to normal’. This stark and honest reflection underpinned Nuno’s entire talk. In a world of constant change (did you know there’s 70 elections happening around the world this year?) we turn to the people we trust for support. This rings true in technology as it does in care. Reiterating Nourish’s focus on building our team to be the right people for the challenge ahead, Nuno painted a picture of a bright, and collaborative future.
Next up was our new Chief Product Officer Matthew Stewart to discuss our new product agenda. Matthew brings a wealth of experience to his role and demonstrated how this is already benefiting Nourish. The talk focused on the key areas of our new product agenda, and how we will be moving forward. Crucially, the session ended with an open Q&A to promote collaboration and idea sharing. Several attendees shared their perspectives and helped further focus the product agenda as we move forward. Co-production is a vital tool for the future development of care, and this is especially true for the development of care technology.
The development of care technology does not have to be a lonely road, as we learned in the last session of our conference. Our Director of Partnerships and Business Engagement Denise Tack detailed the motivation and success of our emerging Nourish Partnership Programme. She was joined on stage by Camascope’s Customer Director Saurabh Shah and PainChek’s Head of Business Development Tandeep Gill. They explained exactly why our Partnership Programme is ‘not just an API hub’ but a collaborative undertaking. One built on a foundation of philosophical and technological alignment. We look for partners whose background, motivation and vision match ours at Nourish as well as their technology.

It was a great day for sharing visions all round. We are deeply grateful to everyone who made the trip to The Gherkin to join us for the day. It was a fantastic time overlooking London Town, learning about our users’ worlds and sharing our plans with them. We can’t wait for the next one, and plans are already in place to hold it in a more northern location so we can engage with our community across the UK.
The day was a reminder of the size, breadth and impact of the community we are a part of, and the joy and purpose we feel working with you.
At Nourish Care we’re committed to continuously improving the accessibility and inclusivity of our technology, working towards our goal of developing a solution which truly works for everyone. We spoke to our Head of Product Design, Kate Horn, to learn more about our approach to embedding accessibility and inclusivity at the heart of our product design process.
“Accessibility and inclusivity have accidentally become a bit buzzwordy in the design world recently,” explains Kate, “and most definitely in health tech design. Why? Finally, we are all talking about ensuring that anyone can access the products we are creating. At Nourish these are not just words, they form the basis of design values that go right to our core, we are person-centred. We believe in a better life for everyone. To achieve this, we need to make sure anyone and everyone can use Nourish.”
“Honestly? They mean quite a lot of different things!
“It is a common misconception that when we talk about accessibility, we are only talking about how we apply colours to designs and how we can make it high contrast. This is a factor, but it barely scratches the surface of the work to be done to make a platform, or an app genuinely accessible to anyone who wishes to use it.
“Hold on a moment though, we are talking here about using something that is in your hand already. We need to take a step back and think about the technology and very basic level of access first and how, as designers, we can get the app into your hand or onto your desktop in the first instance. Given that you are reading this digitally, this is clearly not a problem for you but consider this; in 2022, 13-19 million people in the UK over 16 lived in a state of digital poverty. That means they did not have the tech, skill, or resources to fund internet access on one or more occasions a week.



We cannot just build for the latest and most shiny versions of everything. Accessibility means we need to think about making sure what we create is available to everyone. In a way which does not exclude people, starting at the point of access and empowering them to enjoy the full experience of the platform.
“Inclusive” needs to go even further and it is worthy of a blog post on its own. For now, I want to touch on the importance of ensuring that inclusivity extends to individuals feeling genuinely included, seen and represented within our platforms.
First of all, we aim for the highest possible standard. There is a framework for accessibility in digital design for us to follow called WCAG. Within this there are levels, the highest of which is standard 2.2. This is what we strive to achieve. Standard 2.2 covers everything from the use of text, audio, layout, contrast, colour, platform adaptations, use of imagery, operational considerations, inputs, consistency of design and ensuring the platform is robust. And that’s just to start!
It is a solid start, however, a framework does not go far enough for accessibility and it doesn’t answer the requirement for inclusivity. To achieve this, there are several other elements to consider, starting with words.
Words are a powerful way for us to be both engaging and human, when used correctly. They are also one of the quickest ways for us to disconnect people from Nourish. If we describe areas of the platform or tasks using inhuman or technical language you first have to understand what we really mean and then have to choose if you really want to do it. We’re to make things simpler for you, not more complicated! So, step one for us is to speak in common English and start to create a comfortable experience.



Next on that list is understanding who we are designing for. This requires us to become so embedded in the health and care sector that we are a part of the furniture. Great insight means we understand the everyday challenges the people who are using our platform experience. This ensures we craft experiences for our platforms that work to solve these problems in a way that is comfortable for everyone.
Throughout this blog I have used the words “anyone” and “everyone”. These are crucial terms for defining our approach. Typically, designers aim to design for the bell curve, that is, the biggest group of users.
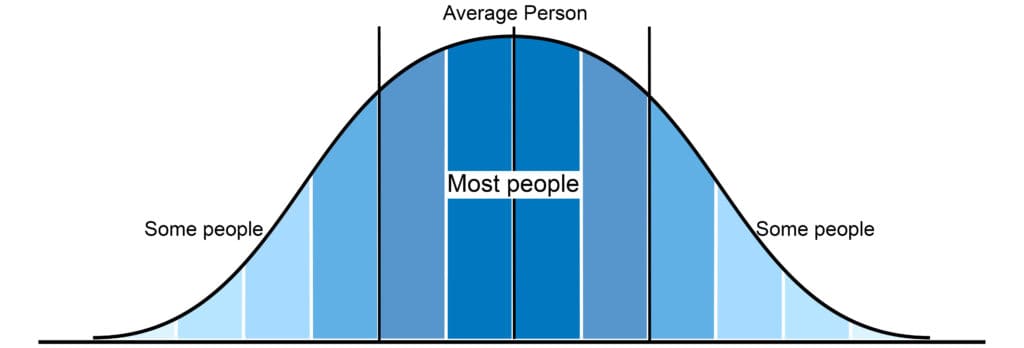
We simply cannot do this in health and social care. We have to step back and design solutions that truly work for anyone. This “flattening” of the curve is really important. It goes to the core of what we work to achieve as a company and the heart of our values as a design team. We want to create technology to truly wrap around the user in a great experience.
As users of Nourish will know, we’re continuously improving the accessibility and inclusivity of the platform, these really aren’t just buzzwords to us. We are working towards our goal of creating a system which can be easily used by anyone. There’s always more that can be done but by keeping these principles and our users at the heart of our design processes we are able to keep our person centred goals firmly in sight.
Book a demo to find out more about Nourish and how we can work with anyone, and everyone in your community.
Thank you to Warrington Community Living for sharing the following article on their website. We love hearing how Nourish‘s digital platform is helping and improving care services across the country!