Social care technology grew rapidly over the past 5 years. A variety of digital and technical solutions for the range of challenges that care providers face every day. In the rush to provide effective solutions suppliers created a new problem, replacing analogue silos of information with digital ones. The Nourish Partnership Programme addresses this problem by building a comprehensive digital estate of integration partners, that our users can review and apply to their service as required, so they can continue to provide outstanding care for their communities.
At Nourish Care we are excited to announce our partnership with Altra, a wellbeing and engagement app. We have covered their activities, wellbeing, feedback and survey features previously. In our final blog we are going to cover our favourite focus of Altra, communication and community.
Altra is an Irish company who were founded in 2019. Their name, directly translated from Gaeilge means ‘nurse’. In this linguistic spirit we would like to share with you another popular Irish phrase; Ar scáth a chéile a mhaireann na daoine. It means ‘People live in each other’s shadows.’ Admittedly something is lost in the translation, but the heart of this message rings true regardless of tongue. We rely on each other for shelter, for strength, for community.
Our family and friends play a crucial role in our lives. When a provider wants to help people to live their lives to the fullest, they must consider the involvement of family and friends, otherwise known as their circle of care. The closer connected someone remains with their circle of care, the more involved and engaged they feel in their own life. Altra gives users the tools to support circles of care, evidence engagement and promote connections on terms that both care providers and the people who draw upon their service can be comfortable with.
The Single Assessment Framework is the Care Quality Commission’s new approach to inspections. The first of the 6 new evidence categories of this framework is ‘People’s experience of health and care services’. In their own words:
“This is all types of evidence from people who have experience relating to a specific health or care service, or a pathway across services. It also includes evidence from families, carers and advocates for people who use services.”
Care providers who engage routinely with the people using their service and their circles of care benefit from a constantly updating record of the experiences of their care. Evidence of which impresses regulators regardless of geography. This information is invaluable for shaping your care, as well as your inspection rating. Altra provides a platform for wellbeing and activities information to be both recorded and shared. One that is rooted in lived experience, regulatory requirements and familial responsibility.
Family means ‘Ohana’, and ‘Ohana’ means nobody gets left behind. This is one of the many key life lessons imparted by Disney’s 2002 classic Lilo and Stitch. A loved one receiving care is a source of great relief for many families, but also one of great stress. The natural impulse to check in on them consistently is one we have all felt towards those we care about. While entrusting your loved one to receive care from a service is a source of immense relief, it is still only natural to want to check in on that service.
Altra makes this process not only simple, but beneficial to all parties. It gives families the tools to share their perception and experience of the care their loved one is receiving with the care provider.
There is an understandable apprehension amongst care providers when deciding how much to involve families and friends in the inner workings of their loved one’s care. The information care providers choose to share with a person’s circle of care needs to be detailed enough to satisfy their questions, while being digestible enough to calm their concerns. Altra provides a suite of features so you can directly link people into a circle of care, clearly illustrate the activities their loved one is engaged with and their level of wellbeing.
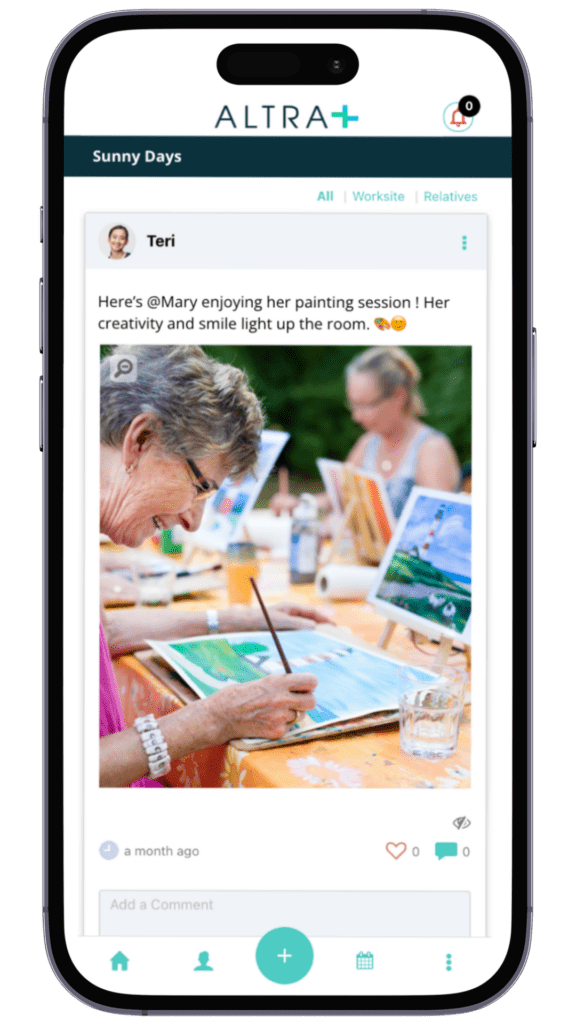
Altra provides a secure engagement application that allows care providers to share updates on the well-being of people utilising their service directly with their circle of care. This app works a bit like an Instagram feed updating the interested party with all the relevant information they need regarding their loved one’s care.
Altra simplifies the process of engaging and collaborating with a person’s circle of care. You can share information with families in a variety of forms, including video, photos and direct messages. Providers use these different formats to paint a complete picture of the support they are providing, and the life the person using their service is living as a result.
This app is not a one-way street either. It promotes engagement by allowing families to post updates for their loved ones as well. Altra enables these digital updates to be easily converted to physical printed newsletters, delighting the people you support. Specific information that speaks to the individuality of the people using your service and promotes the connections that make life worth living.
Altra goes beyond digital connections. Care home operators can use the app to set up ‘family events’. Invite relevant people to the event and it will display who is attending, who has responded and so on. Through this functionality Altra promotes visits in a way that easily feeds back into your existing system. You can include as much information about the planned visit as you want. This simplifies your organisational process while maintaining an up-to-date record of the visit for reviewing and reporting purposes.
Of course, not everyone will be able to visit all the time. You can also arrange video calls through Altra to make sure that residents stay connected to their circle of care.
The app even includes a concierge service. This can be used by the circle of care in a variety of ways, including ordering special requests from the kitchen (such as birthday cakes!) or booking specific outings and events for their loved one. All requests are easily recordable and reportable so you can efficiently factor them into your invoicing process.
Care comes in all shapes and sizes, and it casts a long shadow. One that people, families and communities use for shelter. The more involved everyone feels in the construction of this shelter, the more satisfaction everyone takes in its success. With Nourish and Altra you can build strong connections throughout your service, capitalising on the ones that are already there, and providing the foundations for many more.
You can read more about Altra’s functionality:
Activities and Wellbeing
Feedback and Surveys
Social care technology grew rapidly over the past 5 years. A variety of digital and technical solutions for the range of challenges that care providers face every day. In the rush to provide effective solutions suppliers created a new problem, replacing analogue silos of information with digital ones. The Nourish Partnership Programme addresses this problem by building a comprehensive digital estate of integration partners, that our users can review and apply to their service as required, so they can continue to provide outstanding care for their communities.
Communication drives care. We see this reflected in care interactions every day, as well as the new single assessment framework from the Care Quality Commission. Our ability to understand, to support and to elevate each other is born from our ability to communicate. That’s why we at Nourish Care are so excited to announce our partnership with Altra, a wellbeing and engagement app!
With a suite of features that champion person-centred care, lived experience and wellbeing, Altra offers care providers the tools to transform their communication.
The 2016 Care Act charges providers with the responsibility to ‘promote wellbeing whenever they carry out any care and support functions for individuals.’ A substantial assignment contained in 13 words. The result of this legislation has proven unlucky for some, as the task of promoting wellbeing is as multi-faceted as it is vague.
Outstanding providers know that the best way to promote wellbeing is to promote communication. Involving everyone, from every level of your service, is the best way to ensure you stay connected to people’s wellbeing. Altra empowers users to promote the individuality of the people utilising their service, without significantly increasing the workload on their team or the burden on the people drawing on their care.
Altra gives you the tools to capture pertinent information at the point of care. Carers can post photos, videos and notes within the Altra app to showcase the activities you provide and how people have participated. You can even include polls and tag loved ones, so you get direct feedback from the relevant people. The ability to capture sentiment on each activity gives you a primary source to understand the experiences of your community. This provides an invaluable line of communication to ensure your care is person centred and your people feel valued and listened to.
Altra also appreciates the less time you spend on admin the more time you can focus on communicating with your community. The fluid integration between Nourish and Altra removes the need for duplication of effort. These benefits will be felt throughout your organisation, and Altra really shines when supporting Activities Co-ordinators.
An Activities Co-ordinator plays a crucial role in care homes. On the surface it may seem like a simple enough role. In reality, it carries a depth of meaning and purpose for the people utilising your service We are engaged through action and interactivity. Whether it is music, art or exercise we all have our preferences. What we are really talking about is the act of living, of experiencing the world on our terms and expressing ourselves as people through our actions. An Activity Co-ordinator is an orchestrator of experiences, an engagement conductor, someone who provides those with lived experience of care the experience of living life the way they want, in a place they can call home.
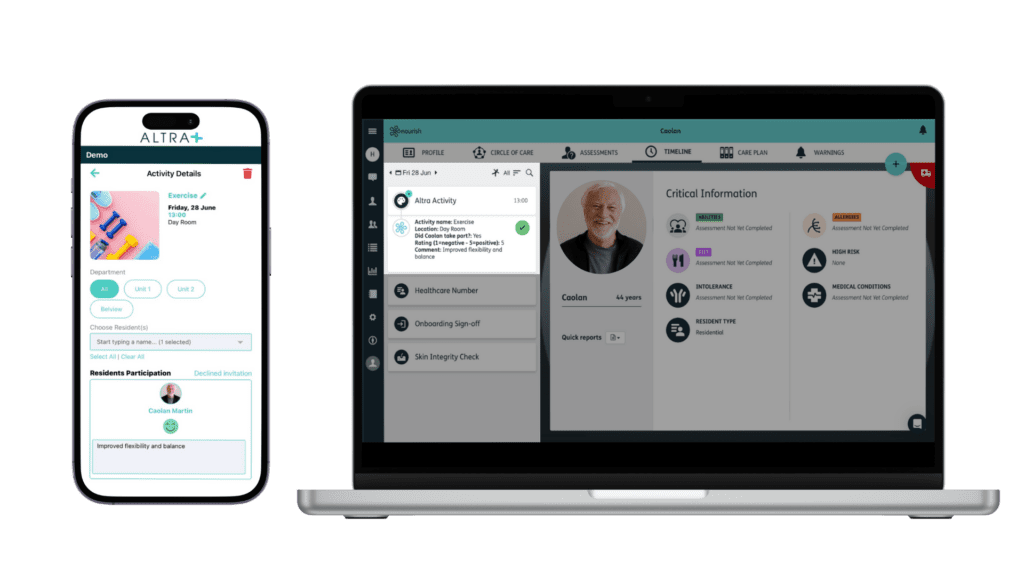
Altra understands this role’s depth and complexity and supports it with specific and intuitive functionality. You can specify your activities, build calendars and review events afterwards to gauge their impact and continuously improve.
Another key functionality that separates Altra from other communication tools is the specificity and customisability of their activities calendar. Simplify your processes with repeating events and the ability to schedule and share your daily and weekly activity calendars in advance. You can store a wealth of useful information in each activity, including start time, attendance tracker, location, colour coding and more. It is easy to keep family members involved with family events and to give them visibility of how their loved ones have engaged with activities through the updates they will see in their Altra family app.
Great activities don’t just fall out of the sky though. Every Activity Co-ordinator has spent a decent portion of their time wracking their brains and the internet for inspiration. Altra simplifies this with a robust and routinely updated wellbeing hub.
This library contains exercise videos, colouring, quiz games, puzzles and more. Don’t worry, this goes beyond just suggesting good ideas for your community. Any additional resources you need for an activity in the library are available to download. Like images for colouring, questions for the quiz or guidance for the proposed exercises from a qualified physiotherapist. Altra gives you the content to put these activities into action, reducing admin and organisation time for your team.
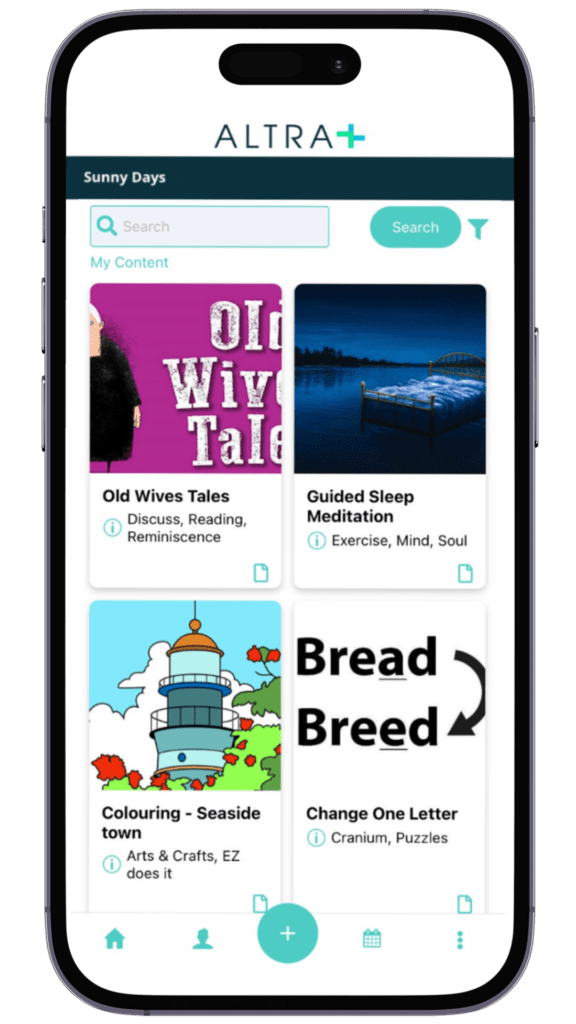
With 1,000s of activities to choose from, which are updated on a weekly basis. There will always be a fresh idea to energise your home and promote wellbeing. Each activity is easily reportable. With the option to engage your team, your community and their circles of care as you choose.
If knowledge is power, then communication is power sharing, and Altra gives you the tools to do both. From your administrator to your aunty, Altra keeps the right people informed. With the right information, to promote the engagement, effectiveness and efficiency of your activities.
You can read more about Altra’s functionality:
Feedback and Surveys
Communication and Family Engagement
Social care technology grew rapidly over the past 5 years. A variety of digital and technical solutions for the range of challenges that care providers face every day. In the rush to provide effective solutions suppliers created a new problem, replacing analogue silos of information with digital ones. The Nourish Partnership Programme addresses this problem by building a comprehensive digital estate of integration partners, that our users can review and apply to their service as required, so they can continue to provide outstanding care for their communities.
‘We need to talk’ – a sentence that sends shivers down spines in bedrooms and boardrooms alike. Feedback acquisition, data gathering, internal research—whatever you name the process, conversation is critical to success. In social care, conversations are a fundamental part of providing quality, person-centred care. Care providers learn the best information about the people who utilise their service by engaging directly with them. Our partners, ImproveWell, build upon this opportunity by offering simple, easy-to-apply engagement tools for your workforce, clients and wider stakeholders.
Knowledge is power and ImproveWell gives you the power to prepare for inspections, increase employee engagement and drive qualified, person-centred improvement across your service.
The Care Quality Commission in England has been rolling out its new inspection process since November 2023. The ‘single assessment framework’ is designed to put people at the heart of the inspection process. While the key categories remain the same; safe, caring, efficient, well-led and responsive, the methods for evidence gathering are updated. There are six categories for evidence that inspectors will now require.
The first three – ‘people’s experience of health and care services’, ‘feedback from staff and leaders’ and ‘feedback from partners’ – are all different forms of conversations. ImproveWell helps your team prepare for these conversations. By making real-time feedback simple and a regular occurrence in your care community by providing a mechanism for feedback anytime, anywhere. You can gain a clearer, and more regular insight into the experiences of your organisation at every level. Without even getting into the results of your engagement activities. Simply introducing the process to your teams and community will make them more familiar and, in doing so, more comfortable with it.
The latter three categories – observation, processes and outcomes – can all be improved through utilising the results of ImproveWell’s functionality. ImproveWell’s solution can be set up in a bespoke way to suit the needs of your team and service. Everyone can suggest ideas for improvement, share how their workday is going, and complete tailored pulse surveys – 24/7. Insights from wider stakeholder groups can be gathered and an AI-powered data dashboard enables group and organisational leads to monitor real-time data, track workforce sentiment, prioritise quality improvement efforts, measure change, and publish reports to complete the feedback loop.
The Maternity Department at Royal Cornwall Hospitals NHS Trust enjoyed notable improvements to their workforce engagement and morale. After the first phase of ImproveWell’s introduction in the Maternity Department. 75% of staff reported feeling able to improve their area of work, compared to the 53% scored by the Trust as a whole. (2018 NHS staff survey) Moreover, over 85% of users of ImproveWell felt it empowered them to implement ideas for change.
This is what makes these tools so relevant to inspections outside of England as well. All inspectors will engage with your staff in one form or another as part of their process. Whether it’s in their ear or over their shoulders. The more familiar the workforce is with being listened to and respected by senior management, the better they can provide and evidence high-quality care.
The Maternity Department at Royal Cornwall Hospitals NHS Trust were able to improve their CQC rating from ‘Inadequate’ in 2017 to ‘Requires Improvement’ in 2018 following their implementation of Improvewell. In November 2019, the Maternity Department won the International Maternity Expo Transformation Innovation Award to recognise achievements made through ImproveWell, and in their most recent inspection in February 2023, they had improved the ratings for ‘Safe’ and ‘Well-Led’ to ‘Good’.
Workforce engagement is crucial in social care. We know that high job vacancies and staff turnover rates are longstanding issues for care providers. One of the surest ways to draw a big audience at any care event is to talk about recruitment and retention. It’s obvious if you have attended any of these talks in the past few years. You will know more and more providers are looking to improve their staff retention rates by increasing their employee engagement.
“We’ve learnt that everyone would like more money but surprisingly it’s not as important as being happy in their work. Support and development of people is held in higher regard.” Residential care provider, Claxton House, Atlanta Healthcare.
The best way to support and develop people is to listen to them. Of course, that’s generally much easier said than done. ImproveWell turns recording, reviewing and actioning ideas from your workforce into a smooth, seamless process. The detail and specificity of ImproveWell’s functionality enables you to ask the right questions. Crucially, the AI-powered data dashboard provides an easy-to-use, insightful overview of the information you have gathered, so you can use frontline feedback for maximum effectiveness. Most care providers conduct internal surveys with their team, with varying results. ImproveWell enables you to take these findings further, and action them to the benefit of your service by empowering your team and wider community to take a more active role in their development, in both a personal and professional capacity.
Health and care providers who use ImproveWell to engage with their community have noticed benefits in four key areas. The first, and most direct benefit, is the increase in staff wellbeing and morale. It is only natural that satisfaction increases and turnover decreases when people feel like they play an active and important role in their workplace.



Users also experience a notable quality improvement, in terms of the care they are able to provide. Primary sources are always the best place to start when looking to improve your processes. It is the people who are directly involved who have the deepest understanding, whether they are providing care, utilising care, or are a member of the community in which you operate. A wealth of insight is unlocked when you empower your community to be actively responsible for their care.
“It’s the quick fixes that make the difference,” Nicole Lee, Chelsea and Westminster Hospital NHS Foundation Trust Burns Service, Burns Matron.
This same logic applies when it comes to your service’s operational and cost efficiency. It is impossible to fully understand something by looking at it from the top down. All leaders know they need multiple perspectives to understand their organisation. Increase your operational and cost efficiency by creating a simple route for innovation. Carers are known for making a little go a long way, harness their ingenuity and experience and the rewards will soon follow.
People are the pulse of our communities. Engage directly with them to best understand the world in which your service exists. The concept behind micro-improvements is rooted in experience and the belief that with the right knowledge, you have the power to change the world. Maybe not the whole thing, but definitely your own. However first, we need to talk.
At Nourish Care we’re committed to continuously improving the accessibility and inclusivity of our technology, working towards our goal of developing a solution which truly works for everyone. We spoke to our Head of Product Design, Kate Horn, to learn more about our approach to embedding accessibility and inclusivity at the heart of our product design process.
“Accessibility and inclusivity have accidentally become a bit buzzwordy in the design world recently,” explains Kate, “and most definitely in health tech design. Why? Finally, we are all talking about ensuring that anyone can access the products we are creating. At Nourish these are not just words, they form the basis of design values that go right to our core, we are person-centred. We believe in a better life for everyone. To achieve this, we need to make sure anyone and everyone can use Nourish.”
“Honestly? They mean quite a lot of different things!
“It is a common misconception that when we talk about accessibility, we are only talking about how we apply colours to designs and how we can make it high contrast. This is a factor, but it barely scratches the surface of the work to be done to make a platform, or an app genuinely accessible to anyone who wishes to use it.
“Hold on a moment though, we are talking here about using something that is in your hand already. We need to take a step back and think about the technology and very basic level of access first and how, as designers, we can get the app into your hand or onto your desktop in the first instance. Given that you are reading this digitally, this is clearly not a problem for you but consider this; in 2022, 13-19 million people in the UK over 16 lived in a state of digital poverty. That means they did not have the tech, skill, or resources to fund internet access on one or more occasions a week.



We cannot just build for the latest and most shiny versions of everything. Accessibility means we need to think about making sure what we create is available to everyone. In a way which does not exclude people, starting at the point of access and empowering them to enjoy the full experience of the platform.
“Inclusive” needs to go even further and it is worthy of a blog post on its own. For now, I want to touch on the importance of ensuring that inclusivity extends to individuals feeling genuinely included, seen and represented within our platforms.
First of all, we aim for the highest possible standard. There is a framework for accessibility in digital design for us to follow called WCAG. Within this there are levels, the highest of which is standard 2.2. This is what we strive to achieve. Standard 2.2 covers everything from the use of text, audio, layout, contrast, colour, platform adaptations, use of imagery, operational considerations, inputs, consistency of design and ensuring the platform is robust. And that’s just to start!
It is a solid start, however, a framework does not go far enough for accessibility and it doesn’t answer the requirement for inclusivity. To achieve this, there are several other elements to consider, starting with words.
Words are a powerful way for us to be both engaging and human, when used correctly. They are also one of the quickest ways for us to disconnect people from Nourish. If we describe areas of the platform or tasks using inhuman or technical language you first have to understand what we really mean and then have to choose if you really want to do it. We’re to make things simpler for you, not more complicated! So, step one for us is to speak in common English and start to create a comfortable experience.



Next on that list is understanding who we are designing for. This requires us to become so embedded in the health and care sector that we are a part of the furniture. Great insight means we understand the everyday challenges the people who are using our platform experience. This ensures we craft experiences for our platforms that work to solve these problems in a way that is comfortable for everyone.
Throughout this blog I have used the words “anyone” and “everyone”. These are crucial terms for defining our approach. Typically, designers aim to design for the bell curve, that is, the biggest group of users.
We simply cannot do this in health and social care. We have to step back and design solutions that truly work for anyone. This “flattening” of the curve is really important. It goes to the core of what we work to achieve as a company and the heart of our values as a design team. We want to create technology to truly wrap around the user in a great experience.
As users of Nourish will know, we’re continuously improving the accessibility and inclusivity of the platform, these really aren’t just buzzwords to us. We are working towards our goal of creating a system which can be easily used by anyone. There’s always more that can be done but by keeping these principles and our users at the heart of our design processes we are able to keep our person centred goals firmly in sight.
Book a demo to find out more about Nourish and how we can work with anyone, and everyone in your community.
Social care is in a state of change. Care providers tasked with being the steady hand through this change have consistently risen to the challenge. Despite having little control over the changes as they happen. At Nourish Care we are embracing this change by working with our users to develop a social care future we are all proud of. With increasing standards, new regulations and extended funding availability it is clear now why so many care providers are embracing change themselves and switching to Nourish.
Care providers have a wealth of options when choosing a digital partner. Under the original standards for the NHS Assured Solutions List (ASL) there are 24 Digital Social Care Records (DSCRs) to choose from. That’s without mentioning the systems who don’t reach these standards. The ASL is enjoying notable success so far, as it continues to work towards its target of 80% of care providers on DSCRs. Digitisation is widespread through social care now. To the point that many care providers are shopping around for a better system to match their service.
The ASL was always intended as a starting point for the digitisation of social care. The Department of Health and Social Care has announced the second step of this journey, with the recent release of the 14 new standards for DSCRs on the ASL. We are one of the few providers to have achieved all 14 of these standards. You can read about the specifics of the standards here.
We are the largest software supplier to have achieved the new standards. As well as being one of the first to get listed on the ASL following its initial launch. Our legacy of forward thinking and innovation consistently aligns us with the future direction of the social care sector. We are proud to be working closely with key decision makers in health and social care.
We support care in a huge variety of settings. Including older person’s care, nursing, home care, learning disabilities, dementia, supported living, assisted living, substance abuse, mental health, children and young people and more. Each care setting is unique, and each care setting requires specific understanding to support effectively.
Our experienced and understanding customer success and support teams will work with you to make sure our system fits your service. Whatever your needs are, and whatever they may become in the future.
Once you switch to Nourish, we are with you every step of your journey. Should your journey lead you to new business opportunities we are the best equipped software supplier in social care to support your expansion. Whether you are focussed on a single type of care or support a range of different needs.
You can also scale your functionality as desired, thanks to our comprehensive partnership programme. The programme unites key best-in-class innovators like Camascope for eMAR, Radar for incident management and PainChek for pain management. All while keeping a finger on the pulse for emerging technologies that will substantially impact the social care sector.
Additionally, we offer more in-depth data packages called ‘Insights’ and ‘Analytics’. These features provide a much richer insight into the data gathered across your service. Perfect for larger care providers who collect vast swathes of information every day, but have no clear way to transform this potential into insightful, actionable information.
The Care Quality Commission’s (CQC) rollout of their new Single Assessment Framework (SAF) is enduring some understandable teething challenges. Initialisms aside the ambition of the project remains clear. The regulator wants to streamline processes and better respond to the needs of the people who draw upon care.
We facilitate these new developments as effectively as possible. We work with organisations like the Care Software Providers Association (CASPA) to share our voice and insights on the development of digital social care with key decision makers in local and national government. Our work on alignment with #socialcarefuture helps to guide the future of our system as much as they guide the future of the wider care communities. Socialcarefuture are the co-authors of the ‘I/We Statements’ that define the SAF scoring.
There is always something new to be considered, a fresh function to be explored or a new piece of legislation to be adhered to.
We cannot know the future; all we can do is prepare for it. We have read the tea leaves, built our houses from stone and made hay while the sun shone. All so we can continue to lead the way in digital social care, through innovation, understanding and collaboration.
Social Care is in a state of change, and with that ever-present uncertainty comes a great opportunity. Switch to Nourish today and take control of your change, with your team, your service and your community.
Teamwork makes the dream work, though a good partnership is hard to find. At Nourish Care we are committed to working with our users throughout their digitisation journey. A journey that continues beyond tomorrow’s horizon and into the future of care. The results of our partnerships are present for the over 385,000 people who are cared for with Nourish software solutions. People define partnerships, and by putting partnerships at the centre of our approach we ensure that people are always our focus.
From the moment you first speak to Nourish there will be someone on our side working with you every step of your journey. This applies to care providers of all shapes, sizes and disciplines.
Digitisation can take time, whether you are looking to reshape systems or just starting off your journey. We make sure all our users have the right guidance alongside them to make this process as smooth as possible for your team and as specific as necessary for your community.
Project managers are available to help care home groups and large franchises transition to Nourish. They work with your team to ensure an effective digital rollout. We have dedicated customer success managers to work with medium and smaller care providers, as well as being another helping hand for large groups. These managers are adept at supporting the unique needs that emerge when providing care for your community. They know how to guide our users during their set-up process to ensure you receive the maximum benefits from Nourish.
Our partnership doesn’t end at the onboarding. We continually work with our users. Offering you an open line and a dedicated point of contact for your service, so you can continue to grow the way you want to and flourish with Nourish. You can read more about how Nourish has supported the teams and growth of home care providers Nexus Care and Priory Group’s care homes.
Visit our Case Studies page for more examples.
Expertise is essential to success, and our partnerships with services excel at combining our knowledge with yours. We have researched and developed robust libraries alongside care and clinical professionals with a deep understanding of the sector and needs of the population. Each library contains interactions, assessments, care plan templates and more for managing specific pathways, conditions, needs and day-to-day operational requirements.
We combine this wealth of best practise and experience with your understanding of your community’s needs. Nourish boasts a depth of customisability. This promotes the individuality of your service in line with the established requirements of commissioners and regulators. The only assets that are not customisable are locked to ensure compliance with a particular protocol or standard. This empowers your coordinators to wrap your system around your service and provide for the specific needs of your community.
There is a reason we are the largest software supplier for social care in the UK. We do not settle for general. Nourish is filled with functionality that supports the unique requirements of different care types. Including residential, domiciliary, nursing, assisted living, learning disabilities and many more.
Strong rostering is the backbone of efficient home care management. We built our rostering with over a decade of experience working with home care providers. It can be set up on repeating schedules of up to a month. Our drag and drop rostering and customisable carer rating system gives you the tools to quickly adapt to changing circumstances with your workforce and the people they support. Your rostering can then be simply invoiced and time-sheeted with our comprehensive finance functionality. Ensuring you pay everyone the right amount at the right time.
Nourish’s mobile app for home care is another product of our strong partnerships with care services. We work with providers to keep our app up to date and empowering their care teams and communities. Carers know where they’re going and what they’re doing, while keeping you up to date on how it went through their appointment notes and audit tracker. Travel times, upcoming schedule, care types, medications and notes are all designed alongside carers and available offline. So your team have everything they need, anywhere they go.
Nourish is designed by care professionals for busy care environments, combining icons, imagery and text to create a smooth, easy experience. Keeping carers informed is crucial in residential settings as well. The care plan summary on our care home mobile app provides a detailed and concise snapshot on mobile for a particular need to ensure nothing gets missed and you have all the information available. Carers have access to all the information on the mobile app which empowers care teams. They can see the handover, review recent and historic appointment notes. A level of autonomy unrivalled by any other DSCR platform. The app also features ‘back’ and ‘save’ buttons wherever you go so no records can be lost when completing a record/interaction.
Data is a hot topic, but one that has burnt the finger of many a service. With Nourish managing data can become a simple part of your daily process. We provide several prebuilt dashboards within our system to provide data oversight to your team. These dashboards can become a cornerstone or a starting off point for your team’s application of data. We have experienced people on our team to help you get what you need from your data in your reporting. So you can focus on providing, responsive, effective care.
All of our success at Nourish has come through collaboration. Collaboration between our teams, between our integration partners and between our users. We believe the best solutions are produced through teamwork. A process without an end, but an enduring, enjoyable journey. We’re in this for the long haul, with true partnerships, the lasting kind.
Many care providers are now looking towards a smarter way of working, and with the recent strain put on the care sector due to the Coronavirus pandemic, it seems now more than ever people will be looking to make the switch to digital.
In this guide to electronic care planning, we map out what the best ways of going about selecting a care plan provider are, and answer that all important question: what are the costs?
Electronic care planning is a very recent and modern market, with most of its current players being fewer than 10 years old. As a result of this, pricing is often a topic of discussion: is it driven by its market, or is the market driving it instead? Is the market mature enough to represent a fair value or are providers offering a round number and see if it sticks? How is pricing calculated – by the number of staff, or people we support? How much is the upfront/setup cost, and how quickly does it start showing a good return on investment? How can I ease off this investment if I am a smaller provider? Can I get support from the Government/my local authority? This guide to electronic care planning tries to answer all these questions and leave you with enough material so that you can set a budget before you start looking for the most adequate ECP for your care provision.
Let’s start with the basics: your budgeting for an ECP is usually broken down in three different types of payments: Licensing (recurring costs), Implementation (one-off initial costs) and add-ons (additional costs if there is a variation from the initial requirements).
1. Licensing: this is your subscription cost which will be the bulk of your budget; it should cover the usage of your solution, any server costs, security, backups, support, account management, and product development.
????Tip: Always ask if the list above is included in your licensing cost. Nobody likes being surprised with a lower licensing price only to find out later that support or account management are add-on.
2. Implementation: this is your initial setup cost, which is usually roughly the equivalent of the first year of your licensing cost. It should cover any hardware, training, and setup fees.
????Tip: Some companies might offer you implementation at a very low cost, or even for free. It’s
good to bear in mind that this may indicate that a company is relatively young and might not be as
robust as other, more mature providers.
3. Add-ons: Anything outside of the scope of the initial plan would fit this category. For instance, if you expand to get a new unit, require a couple of additional pieces of hardware, or require additional training, you should expect there to be a cost for these.
????Tip: A transparent company will always be clear about any add-on costs. Be cautious if any Licensing or Implementation cost mentioned above fits into the “add-on” category, since you should expect them as standard.
Usually the cost represents a breakdown of the points mentioned above: the usage of the solution, server costs, security, backups, support, account management, and product development. A lower cost usually means some of these key elements is severely reduced or even not included.
Another important point is understanding whether the solutions is fully cloud-based, on-premise, or mixed. Most modern ECPs are fully cloud-based, which should be your preference: it will be much more robust, future proof, with regular updates, and you will be able to access your care records from anywhere (with the right permissions).
On-premise solutions usually have a higher implementation cost and require higher add-on fees when there is a maintenance problem. Cloud-based solutions are usually more expensive initially but being future proof, you are not surprised with hidden fees and required upgrades at any point.
????Tip: ask the following questions to understand if the service will be within your expectations:
1) How often is the system updated with newer, better features and clinical updates from the sector?
2) Who receives support, how is it offered, and is it 24/7 all year round?
3) Is the data stored in the UK and how often are backups conducted?
Our guide to electronic care planning will break down the different types of licensing you can get. You will most likely encounter one based on the number of people you support, one based on the number of staff you have, and one based on the number of devices you are using.
1. Based on the people you support: this usually gives you a fair price because it’s directly based on your revenue.
????Tip: some providers offer you discounts based on different brackets so try to use that to your advantage. Also, clarify whether this impacts the capacity or occupancy of your numbers
2.Based on the number of staff you have: roughly a similar cost to the one above depending on the ratio of staff to people you support.
????Tip: ensure you have enough accounts for every member of staff or you will start losing accountability if people start sharing accounts. It might save you a very small cost initially, but it can have dramatic impact in evidencing care on a later stage.
3.Based on the number of devices you are using: usually more common in legacy ECPs, you will only pay for how many devices you require. Usually a good option if you have a low ratio of staff to people you support.
????Tip: Same as above, ensure every member of staff has access to the ECP at any point in time. If you neglect this, the ECP can become a downgrade from paper, since there will be times where staff will have no access to care plans, or no way of evidencing their care.
As with any decision, this will have an impact on your business. You should look at your options, even once you have picked your favourite ECP. Our guide to electronic care planning provides some ideas for how you can mitigate the implementation cost to a minimum:
1. Can you do one or more training days remotely? Usually the cost is reduced in this case, and there are many benefits such as multiple people being able to join, the ability to record the session and reuse it in the future, and ultimately best use of time. With the world adapting to the spread of Covid-19, this is likely to become the norm for many.
However, try keeping remote sessions only to staff who is comfortable doing this – and support staff struggling with technology with face to face training.
2. If you have more than one home, try joining the senior staff together, cutting the cost in half. The more homes you have, the more cost efficient it can be. But bear in mind too many might shift a workshop environment to a less practical “classroom” approach which might not be ideal.
3. Look into alternative hardware options. Cheaper hardware usually means more headaches in the long run, but if you have a strong policy for hardware handling in place, it might be worth looking at all the options.
4. Financing is another option – ask your ECP provider if they can recommend anyone or do your own research if you’re more comfortable doing so. It’s not unusual to see single Care Homes splitting the implementation cost across 12 or 24 months.
Picking an ECP is invariably a decision to which Care Providers say “I don’t know how I did not do this earlier” since it’s one of the quickest returns for a business which relies so heavily on data. You can split the benefits into tangible (direct saving in cost) and intangible (indirect saving in cost) savings. When you take notice of intangible savings is when you truly realise the advantages of an ECP.
1. Tangible savings: stationery, paper, printer leasing, printer ink, files, binders, pens, you name it. Any expense you currently have with paperwork is almost immediately reduced to almost zero. Archiving is another factor you will realise in the mid to long term: whether you store your archived paperwork in a shed, your attic, a room, or externally with a storage company, this is either direct capital or an asset that you will be saving: usually this means you will either make significant savings or be able to have an extra room in your care setting.
2. Intangible savings:
Adopting an ECP is not a question of if but when. More and more care providers are adopting ECP, which is giving them a business advantage over other providers who are still reliant on paper-based records. More emphasis is being placed upon the value and benefits ECP can provide, with even the likes of inspectors and commissioners endorsing using this approach to recording care. Take advantage of this by comparing the already mature ECPs in the market since it’s not a new sector anymore, and you will quickly reap the benefits described in this article.
????Tip: reflect or measure how long it’s taking your senior team to do audits, reporting, and staying on top of care plan reviews. This should be a great foundation for how much you will be able to budget in your decision. Repeat the same exercise for your costs on staff recruitment, retention, and overall happiness in writing paper notes every day.
????Tip: When picking an ECP, prepare your meeting well by setting a list of criteria you are looking for by including not only required features but also what is included in the cost breakdown. The better prepared you are, the less hidden fees will surprise you.
????Tip: Moving to an ECP is a massive business decision. Ask your peers, local providers, and communities for a reputable provider rather than being driven purely by cost – cheap is not always best.
????Tip: Do not neglect the quality of Support and Account Management. An ECP requires a significant process of change management in your care provision, so think of it as a journey and never as an end goal.
To download this guide as a PDF, click here. If you’d like to find out more about what Nourish can do for your electronic care planning needs, then drop us a message or book a demo today!
The CQC is starting to recognise the importance of technology within social care and is actively pushing the benefits of a number of technologies such as telecare, telemonitoring, mobile health and digital records. This includes the likes of electronic care planning with a platform such as Nourish. But how a more efficient care management system boost your CQC ratings? .
Going digital is quickly becoming the norm in the care sector and for good reason. Efficiency, data protection and compliance are just a few of the things that make electronic care planning desirable to many care providers. And while they are not currently mandatory within the care sector, they do have a significant chance of boosting your CQC ratings.
What’s wrong with our current way of working?
Nothing. Many care organisations are very happy with their existing structure and processes, but it’s the paper-based system that’s slowing them down. There are plenty of organisations who have good or outstanding CQC ratings even with a paper-based system, but an electronic care planning system can help you achieve these scores quicker and easier, so you can actually focus on giving person-centred care rather than feeling like you’re always filling out paperwork purely to meet CQC’s expectations.
Having everything recorded in one place can make audits far less stressful, and as the CQC also start to realise how much easier it is to complete an inspection when everything is managed electronically, making the switch to a digital way of working seems the natural way forward.
But electronic care planning isn’t about changing the way you work, it’s simply about using a different platform to enhance your current way of working. At Nourish we designed a totally flexible platform that can be moulded to suit your current way of working, not the other way around, while allowing you to reap the communication and responsiveness benefits of managing information digitally.
No matter what type of care you are providing, whether it be residential care for older people, support for people with learning difficulties, mental health, dementia or other, Nourish’s electronic care planning system can help you focus on the people you support rather than paperwork.
Isn’t it just the same as what we do now, but on a computer?
Electronic care planning can be so much more than what it says on the tin. Some electronic care plans are quite literally just digitally recorded care plans, the same as they are on paper. While these do have some benefits, in order to see changes in efficiency, you need a platform that is going to refine the way you already do things, so that it’s quicker, easier and clearer for carers to use.
In order to use electronic care planning to improve your CQC ratings, you don’t necessarily need to change the way you provide the care, only the way you record and evidence it. Electronic care planning can offer different ways of doing things that allow you to stay focused on person-centred care, most importantly, it can allow you to have more face-to-face time with those you support rather than spending time on lengthy paperwork.
Nourish is an innovative platform with ever-evolving features that can help you provide better daily care outside of the electronic care plans. So whether you already have an effective structure in place or you’re looking to improve the way you do things, Nourish’s electronic care planning system has a lot to offer.
Transparency of Care is Key
We believe transparency and consistency across care teams is essential when it comes to achieving good and outstanding CQC ratings. Nourish is designed in a way to encourage clearer communication to empower carers across the sector.
We want to help you provide the best quality care in the simplest form. Rather than try to create something very complex, we have kept the user interface clutter free and the features limited to the things you need. Care plans are one of our most-used features, however there are many other features which have proven to be incredibly useful when it comes to meeting CQC standards.
How electronic care planning can help
Nourish has a number of unique features that can help you build a more effective care management system and boost your CQC ratings. Here’s just a few…
Seamless handovers
Nourish’s handover feature is one of the main ways we encourage transparency across care teams. If one of your members of staff comes back after a week or two of holiday, catching up can seem impossible with a huge pile of papers to work through. This is where things can get missed and your CQC ratings could slip.
The handover feature allows you to view the past days and weeks all in one place, and easily pick out any important notes that may have been recorded in your absence. Carers can leave specific handover notes for those who are absent, and these are then there for when they come back to work. It’s also the perfect tool for ensuring everyone knows what’s happening at the changeover of shifts, so someone starting the night shift will be able to clearly see everything that’s happened throughout the day.
These notes will also be visible in the relevant sections and can be viewed when recording at the point of care and can also be read easily by a CQC inspector and evidences the clear communication within the team
Body maps
Skin conditions are usually monitored and recorded on paper, which means that when changes occur (which they can do frequently), it can be difficult to update the records quickly enough to pass this information on to a wider team. The body map feature allows you to report on new and existing skin conditions at the point of care, creating a clearer flow of communication and reduces the risk of mishandling of those who do have certain conditions.
The transparency that this feature ensures that everyone is equipped with the relevant information to do their job safely and effectively, and with everything recorded on the body map within the Nourish app, when it comes to a CQC inspection, there is clear evidence of how you manage this.
Scored assessments
Nourish’s scored assessment feature allows you to closely monitor those you’re supporting in order to provide the right kind of care. By answering a series of questions, Nourish can then generate a score and create alerts for certain things so that carers can react quickly to change.
This provides a more accurate way of tracking things such as nutrition, fluid intake, behaviour, wellbeing and more, so that you can provide care that is completely tailored to the individual’s needs.
With a slicker, smoother way of creating care plans, recording notes, and managing staff, everyone benefits from electronic care planning. Not only are people receiving more person-centred care, but carers feel empowered by the open communication and clarity surrounding care plans, which ultimately makes for far more efficient management within the care sector.
No matter what your current CQC rating, the Nourish system can help you improve your overall efficiency, saving you time and stress when it comes to those all-important CQC inspections.
Those details that make your care team stand out and life more colourful
When care teams have the right culture and values and the time to focus on each person, this becomes visible in the little details: receiving personal care according to the individual’s preferences, finding what is meaningful for each person and enabling each and every one to have aspirations.
Whether that’s watching the cricket, feeding the ducks or checking the grandson’s new update on Facebook. Being able to demonstrate how your team goes above and beyond to help each person they support find meaning and wellbeing every day is a big part of what moves the needle towards the coveted Outstanding rating.
And Nourish enables exactly that do be done simply, by configuring each interaction so it’s aligned with personal preferences, or by recording ad-hoc interactions on the go, with photos, voice annotations recorded by your team or the person themselves. It’s the ultimate demonstration that each person is living a fulfilled life, above and beyond being kept safe, their life has meaning, and the care team is able to innovate every day to improve the wellbeing of those they support.
New technology in care is revolutionising the way we support people and artificial intelligence is quickly making an impression on the social and health care sectors. From the latest smartwatches recording our morning runs to electronic care planning systems and even robot surgery! New innovative tech systems and devices are collecting data and analysing trends to identify patterns, and cross-referencing patient data in order to gain quick and reliable insight. While some are celebrating AI’s ability to revolutionise the way we care, many still fear this technology and see it as a threat to their personal security, something we have looked at previously ‘Electronic Care Planning: Change Doesn’t Need to Be Feared’
A large part of this fear is down to education, and in order to encourage not just care professionals, but anyone and everyone who interacts with the world of care, to have confidence in these technologies, it’s important to highlight the great benefits that they offer to the lives of those we love and care for.
In this article, we’ll be looking at some of the latest technologies that are enhancing the world of care management through data analysis and the well-being of those in care.
One of the new technologies we are seeing revolutionising the way we care is Virtual Reality (VR) headsets, which could soon become standard in dementia care homes. More than just a form of entertainment, some recent small studies suggest that VR environments could help trigger old memories in seniors, helping to make them feel less alone and confused.
Not only does this have positive effects on those living with dementia, but it improves their relationship with their carers and families too. It can reduce aggressive behaviour in patients and allows carers to gain better insight and understanding of those they’re caring for, thus improving caring interactions.
The FDA has recently approved the first version of a Glucose Monitoring System, which can be implanted just below the skin and has a sensor that can be worn for up to 90 days. These systems continuously monitor sugar levels and send data to a display device, and they also allow you to set up alerts for high, low or significant changes.
This will allow carers to monitor those with chronic diseases like diabetes much more closely, including during the night, and they can track trends in changes to sugar levels. A CGM also reduces the need to do finger prick tests and allows you to administer more accurate doses of insulin. Ultimately this device enables carers to act quicker and care better.
5G is quickly changing the efficiency of social care. With analogue signals soon to be switched off, 5G will allow much faster, safer and more reliable handling of data. 5G offers speeds up to 10 x faster than 4G, and it’s being used in a number of ways to provide support, including remote monitoring.
Remote monitoring can benefit elderly or vulnerable groups who receive care as it can reduce the number of trips they need to take to the hospital. Care professionals can receive and analyse data, as well as share data securely and in real time. Devices powered by 5G could help carers detect problems earlier, and refer and exchange data with other care professionals for more accurate and better quality care.
Smart technology has been on the scene for a little while now, but it remains one of the leading technologies revolutionising the way we care. Homes are kitted out with everything from smartphones to energy meters and assistive technology like Alexa or Google. And this is no different in a care environment. Carers are quickly beginning to adopt a digital way of working, using electronic care planning systems (like Nourish), to enhance the way they care.
Many organisations in the care sector are now seeing the benefits of going paperless. Not only is it more environmentally friendly, but it allows for far more accurate data capturing, recording at the point of care, and most importantly, more person centred care because staff are no longer having to take hours doing admin tasks.
While many of these technologies may still seem like something from the distant future, 2020 is seeing a far more encouraging approach to integrating into the world of digital, with some of these things already being used by social and healthcare professionals.
Technology in Social Care…
Since Kate Terroni became Chief Inspector this Summer, I have been reflecting on how a new person in that post would see their role in promoting innovation in the care sector. It was with childlike excitement that I read Kate’s latest blog post. In this, Kate describes how she has been shadowing some of her inspectors and her findings – and it was fantastic to get her initial thoughts on the use of technology by care teams.
“Speaking with carers I have found that this technology means they can spend more time with the people they support and less time doing paperwork — a welcome benefit of technology.”, Kate Terroni, Oct 2019
And what is the most refreshing is the clarity of thought on the difference between “using technology” and “innovation”, something that resonates immensely with how we see the world at Nourish.
We have long been believers that carefully designed technology, with the right associated services, can enable a whole range of cultural changes. Including how care teams perceive their own ability to drive innovation. It is important that care teams don’t develop a perception that innovation is something you buy. It is not.
Care teams showing CQC what good technology can achieve is a wonderful demonstration that technology makes a difference for them. It hasn’t always been this way.
Going forward it’s important to acknowledge that for a long time, many people misunderstood the potential for technology in Social Care. With a dozen challenges constantly putting pressure on care teams, the prospect of making a big change such as embracing digital tools for managing care has often filled people with dread – which is very understandable. And historically it wasn’t just for fear of change that care teams have put this off.
The maturity of the products available has come a long way in the last 5 years. Prior attempts to adopt technology by care teams invariably resulted in frustration – products that looked amazing in the eyes of a manager or the owner of a care home ended up requiring hours of training for care workers with clunky user experience, poor customer support, resulting in failed uptake, and a background feeling that “technology doesn’t work in social care”. Care workers were never heard in the process of choosing digital tools, and the introduction of technology was often done in the assumption that it would “help the numbers by making carers more efficient” – as if efficiency could be introduced by some sort of industrial process of optimisation. Thankfully, the sector and the technology that supports it have moved on.
Like any context that is as complex and nuanced as social care, the thought of designing technology at arm’s length resulted in oversimplified solutions often shaped within a software team which would then sell it as fast as possible – this was never going to work. So, what is it about social care that is so different from, say, healthcare? Why can’t we just use a personal health record and expand it?
Well, we can’t. We can’t because social care is not just about someone’s condition or frailty. Good social care services support the person as a whole. And people are extremely diverse – society as a whole is learning that there is no such thing as a template for an “older person” – as we have more people living longer our cultural stereotypes of what is an “older person” are crumbling – older people are “people” – we can’t stereotype them. And therefore, there is no universal template for an Older Person’s Care Plan. Good social care for a person living with frailty supports the person in a way that is aware of the whole person – not just of their frailty. And whereas a person has dozens of encounters with healthcare services in a year, the same person may have dozens of encounters with their care team in a single day.

Care Plans are as diverse as the people they are designed to support.
So, having spent 6 years continuously co-designing Nourish with hundreds of care providers, it’s no surprise care teams feel so different about us. We are not a “technology” company. We are a company that uses a software product and services to make care teams feel empowered to improve and innovate in the context of the care they provide. Carers don’t need to sit on training sessions for hours, it’s intuitive technology that allows them to understand the context of a person, know how to support and what’s important for the person, record naturally as part of providing support rather than “doing record keeping at the end of the shift”, and feel empowered. Empowered because they can spend more time with the people they support. And in addition, from knowing their residents better, they can continuously innovate, suggest adjustments to support plans, identify shifts in personal preferences or suggest new activities that are likely to improve the quality of life for each person.
Innovation happens when care providers design new and better ways to discharge people from hospital, or when they find different ways to enable people to go on a holiday, fulfil a last wish, increase their comfort, find or revive a sense of purpose, supporting every person, old and young, to be and feel the best they can feel.
Technology that enables care teams to do this, will be at the heart of all good care teams in the future. And we are delighted to see the Care Quality Commission so clearly sharing our vision on this.
Could technology help your care service?
Find out more about whether using an electronic care planning could help you and those you support here.