Artificial intelligence (AI) has shifted from a niche topic in tech circles to a headline conversation across health and care over the past couple of years. What was once the preserve of data scientists and software engineers is now discussed in care home corridors, home care offices, and even over the dinner table! But while the hype is loud, the reality for social care is more nuanced, filled with both opportunity and the responsibility to get it right. Join us as we explore the reality and potential of AI in social care.
Much of the buzz stems from Generative AI (GenAI). Tools like ChatGPT and Microsoft Copilot that create new content like text or images. These have made AI accessible to anyone, even those with no technical background. This accessibility has sparked imagination and curiosity across the care sector. Care leaders are starting to ask, “What can AI do for us?”
However, the reality is that large-scale return on investment (ROI) for AI in social care hasn’t been fully realised yet. While the tech industry is racing ahead, the challenge for our sector is not to chase AI for its novelty. But to apply it deliberately to real business and care problems.
Two clear paths exist:
For obvious reasons, at Nourish we believe it’s the second path that holds real promise for social care.
At its best, AI offers a way to augment human work, not replace it. In social care, this means easing the administrative load, surfacing critical insights faster, and supporting preventative approaches that improve quality of life for the people we serve.
A useful way to think about this is through the ‘Triple Aim’ framework from US healthcare, which focuses on:
For UK care providers, AI can directly support these aims. For example:
Crucially, this is not about replacing carers with algorithms. It’s about using AI in social care to lift some of the cognitive burden. So that staff can spend more time doing what only humans can. Building relationships and delivering compassionate, intuitive care.
AI depends on data, and in social care, the ongoing shift to digital systems means we now have more data than ever before. Care records, care notes, health metrics, and incident reports all hold valuable insights if we know how to extract them.
Two main AI techniques are particularly relevant:
The most effective approach blends these techniques with expert oversight. A concept known as supervised learning. This ensures the AI’s “understanding” is guided by the experience of clinical professionals and frontline carers. Which in turn ensures the insights it produces are safe, relevant, and trustworthy.
Social care deals with some of the most sensitive data possible, and the wellbeing of real people. That makes Responsible AI not just an ethical choice but a practical necessity.
Responsible AI follows core principles:
This last principle is crucial. In social care, AI should suggest, not act. That is what we mean by augmenting, rather than replacing care. A falls-risk prediction, for example, should prompt a human review and intervention. As opposed to automatically changing a care plan.
This protects against the risks of over-automation. So, providers can ensure that the irreplaceable human qualities of care, empathy, intuition, and contextual judgment, remain at the centre. This is why we build systems that are transparent and auditable. So, we understand why recommendations are given and remain accountable to them.
Responsible AI opens the door to several promising use cases:
These examples share a common goal. Namely: moving from reactive care ‘What happened?’ to proactive and preventative care ‘Why is it happening, and how can we change the outcome?’.
For AI to be embraced in social care, trust must be earned and maintained. This means:
Trust isn’t a one-off achievement. It’s a relationship that must be nurtured through ongoing transparency and collaboration.
The potential of AI in social care is undeniable. Used responsibly, it can improve outcomes, reduce costs, and allow carers to focus more on human connection. But the key word is ‘responsibly’. Rooted in human experience and shaped by the people and communities it supports.
The most effective AI in our sector will come from co-production. Solutions developed hand-in-hand with those who understand the realities of care and support. Both in terms of those who provide care and support, and those who utilise it. This ensures the technology supports the real needs of the sector. Rather than forcing the sector to adapt to the technology.
In the end, AI in social care should not be about replacing human judgment but empowering it. The goal is a future where technology enhances the compassion, skill, and dedication that define our sector. Where AI is the assistant, and people remain firmly in charge.
Our Chief Marketing Officer Lee Gilbert recently joined David Thompson and Natasha Bone of Rehability Care for a two part episode of their podcast, Social Care Chronicles.
‘Digital Care Planning in Action: Transforming Lives with Nourish’ explores how we are working with our users to reshape the future of social care.
Part 1 of the episode covers a range of topics from reducing paperwork to empowering individuals with learning disabilities, autism, and mental health conditions. Our conversation uncovers the real-world impact of person-centred, data-driven care.
You’ll learn
Whether you’re a care provider, tech innovator, or policymaker. This episode is packed with insights on digital transformation in social care.
Don’t miss Part 2, where we dive deeper into implementation, integration, and what’s next for the future of digital care!
Part 2 premieres at 11:00 A.M. 10th September 2025.
In Part 2 we explore
Learn more about the innovations at Nourish. And how we’re building for the future of social care on our Articles page.
In health and social care, incidents, such as clinical errors, safeguarding breaches, or behavioural events, can have far-reaching consequences. The immediate concern is always the safety and wellbeing of the individual receiving the care or support. An aspect of incident management we explored in a previous blog. However, the impact on care and support providers themselves is equally significant and often under-recognised. A comprehensive overview and specific understanding of incidents in health and social care is vital for keeping managers informed, providers successful and people safe at every level. More than that, with the right application and culture, incidents become a tool for learning. Turning consequences into learnings, and stubbed toes into forward steps.
An incident in a care or support setting is more than a momentary disruption. It can trigger a series of operational, emotional, and reputational challenges for providers. Staff may experience stress, guilt, or fear of blame. Highlighting the importance of the work they do, and the responsibilities they bear every day. This emotional toll can lead to burnout, reduced morale, and even staff turnover, further straining already stretched services.
Operationally, incidents often require immediate response: investigations, reporting to regulatory bodies such as the Care Quality Commission (CQC), and implementing corrective actions. These processes demand time, resources, and leadership focus. Potentially diverting attention from day-to-day care delivery. For smaller or independent providers, the burden can be particularly acute. Where the ability and time to adequately record, review and address incidents simply isn’t available. Especially if incident information needs to be recorded in siloed, separate systems.



Beyond the recorded incidents there remain the ‘near misses’. Minor issues that are not reported because people do not recognise their significance or have the time to record them. These are valuable insights often lost to inefficiency. When we are trying to build a complete picture of someone’s life all the pieces matter. There is no room for uninformed assumptions in preventative care and support.
When talking to care and support providers, we frequently hear about the same challenges. Managing incidents and learning from them is fantastic. However, it is quite challenging to do with siloed information. There simply isn’t the time or system to bring these benefits into the same pathway. The benefits of effective incident management are obvious, but the realities are demanding. Investigations require context, and when so much of what you know about someone is held in different places, that context becomes time-consuming to gather.
Another challenge we discussed focused on evidencing. With regulators, if all they see is a lot of incidents recorded without evidence of responses, they generally view that as a negative. ‘You have a lot of incidents, why is that?’. Quality evidencing demonstrates the quality of your incident management. It became clear that reporting incidents can be a hugely positive thing, if you can demonstrate your response and the learned outcomes. The ability to link incidents to action plans creates a clear understanding of how you are supporting the people utilising your service.
As it stands, this is quite a costly undertaking. In terms of both people and time. Throughout our conversations, we felt it was possible to embed incident management in the care management process at an organisational level. Simplifying processes by building functionality that supports best prastise, and highlights learned outcomes.
The NHS Patient Safety Incident Response Framework (PSIRF) encourages all care providers, including those in the private sector, to adopt a systems-based approach to incident management. This means moving away from blame and towards understanding the root causes of incidents whether they stem from human error, systemic issues, or gaps in training.
Of course, understanding is easier to desire than attain. Finding the information, the insight and even just the time to review your incidents can be challenging in a health, care or support setting.
Many care providers face common challenges as a result. Such as a lack of efficient and systematic investigation and learning process. This can lead to difficulties actioning and evidencing learning outcomes from the incidents. Which in turn negatively impacts your service’s ability to upskill teams, identify patterns and plan for the future.
Embedding a learning culture not only improves safety outcomes but also empowers staff. When care workers feel supported to report concerns and learn from mistakes, the entire organisation becomes more resilient and responsive. Additionally, when the benefits of your learning culture become clear, the buy-in from team members increases significantly.



A learning culture often starts as an abstract idea. One that must be pulled from the ether through commitment and effort. Which is an awful lot to ask from any health, care or support service!
The right partner can help you to create a feedback loop of information. Effectively an engine on continuous improvement that operates alongside your service. Informing your team at every step, while being routinely updated.
Well-designed incident management software helps care and support providers to establish this habit. Well documented and easy to navigate incident reports can be folded into your processes. So, they naturally become a part of your service, from incident, to report, to response to learnings. The accessibility of this information directly influences their impact. It is much easier to include incident notes in a review session when they are available at the click of a button rather than buried in a series of filling cabinets or spread out across multiple siloed systems.
Crucially, this information builds upon itself over time. Unlocking foresight for your service by establishing and updating trends in your community.
The ability to monitor the present, understand the past and prepare for the future is the key benefit of taking advantage of your care data. With incidents and effective incident management software, you can take control of your data to better support your community from start to finish and back round again.
Incidents in health and social care are not just isolated events, they are signals. For care and support providers, they offer critical opportunities to reflect, learn, and improve. With the right partner care and support teams can use incident management tools to increase visibility amongst their managers, building confidence in their actions and a library of evidence for regulators. An impact on your service that ripples out throughout your whole community creating a culture of proactive action. One that delivers better results for the people utilising your service, better impact for those providing it, and better business outcomes for you.
Learn more about how Nourish can help you make the most of every ‘incident’ you have with our upcoming incident management system; Nourish Safety.
Care and support is always evolving. Medical advances and demographic changes mean that established practices require frequent review. With rising demand, increasing complexity of support needs, and a workforce under pressure, providers are being asked to do more with less. From care and support staffing to funding, providers are feeling the pinch, and the sting goes down the line to the people they support. Fortunately, technology is always evolving too, and in some co-produced cases, it’s helping support solutions.
At the heart of the workforce challenges facing social care lies a simple truth, you can’t staff effectively if you don’t understand the needs of the people you support. That’s where dependency assessments can make a big difference. By systematically measuring the evolving needs of the people supported, providers can make informed care and support staffing decisions that are both efficient and person-centred.
Care and support staffing isn’t just about numbers. It’s about matching the right skills, at the right time, to the right people. Yet, many providers still rely on static staffing models or gut instinct to determine how many team members are needed on a shift. This approach can lead to overstaffing during quiet periods or, more worryingly, understaffing when needs are high.
This issue is particularly acute in elderly care, where residents’ conditions can change rapidly. One resident recovering from surgery may need intensive support for a few weeks. While another with progressing dementia may require increasing supervision and emotional care. Without a clear, up-to-date picture of these needs, care teams are left to react rather than plan. An issue that presents itself both at the point of care delivery, and in the head office.
The UK’s social care sector is already under immense strain. As of 2024, Skills for Care research showed there were over 131,000 vacancies in adult social care in England alone. With recent government decisions to significantly reduce overseas recruitment for care staffing, the pressure on domestic recruitment intensified. In this context, making every staffing decision count goes beyond good practice. It’s a matter of survival for both the person drawing support, and the business providing it.
Let’s take for example, a mid-sized care home in the Midlands. The manager noticed that her team was increasingly stretched during the evening shift. Complaints about delayed assistance were rising, and staff morale was dipping.
The manager decided to trial a structured care and support assessment for one resident who had recently returned from hospital after a fall. The assessment revealed that the resident now required assistance with mobility, toileting, and medication. Needs that had previously been minimal.
This insight prompted the manager to adjust the evening rota slightly. A change which ensured a senior carer was available to support the resident during peak hours. As a result, the resident received timely care, staff felt less overwhelmed, and the overall quality of care improved.
The assessment opened a new perspective on the needs, and the resources, of the care community. It allowed the manager to better understand both their team and their resident.
Crucially, the care and support assessment didn’t just help one resident. It highlighted a broader issue. The home’s care staffing model hadn’t kept pace with residents’ changing needs.
What the manager discovered with that specific resident was just the tip of the iceberg of what a level of need assessment tool can unlock in care and support settings. When we widen our scope to a whole service we can see the potential impact increase significantly. The right digital tool will help you track the support and staffing needs of your service with accuracy and efficiency.
You can also improve your team’s satisfaction by reducing burnout and ensuring fair workloads with more efficient care and support staffing. All of which feed into the efficiency, effectiveness and understanding of your service. Enhancing care quality by ensuring residents received the right support at the right time, from the right people.
This is the power of measuring care and support needs at scale. It transforms care and support staffing from a reactive challenge into a proactive strategy.
Transparent, data-driven tools can make a huge difference. Designed to help providers track and visualise the evolving needs of those they support. The best systems offer a clear, real-time picture of care and support levels across a service. This empowers managers to make confident, data-informed decisions about staffing, care and support planning, and resource allocation.
Unlike traditional paper-based assessments or ad hoc reviews, dynamic, data-driven systems can integrate fluidly into daily workflows. We know it’s not just about ticking boxes, it’s about creating a culture of responsive, person-centred care.
Knowledge is power and siloing the knowledge you have available to you drains the power of your service. Integrations build connections across your systems to centralise your information and expand your perspective. When your level of need system can talk to your care management system, it is able to inform your care plans. This creates a comprehensive and accessible picture of the people utilising your support. Ultimately helping to drive improved outcomes across your service.
Connections continue to define care and support as the sector digitises. Much like the crucial connections in your community, the connections in your technology rely on open communication. This is the key benefit of integrations and a core focus here at Nourish. If you are looking to further digitise your processes there are a wealth of options for a range of functions. Picking systems that integrate helps you avoid replacing a physical filling cabinet with a digital one. Instead giving you a robust, interlinked digital ecosystem to support your community. If you’d like to learn more about partners Nourish integrates with check out the Nourish Partnership Programme.
In a sector where every minute and every resource counts, understanding the needs of your community isn’t a luxury, it’s a necessity. Care and support assessments provide the clarity needed to make smarter staffing decisions, improve outcomes, and support your team. From the quality of life of an individual utilising your service, to the overall efficiency and viability of your businesses finances!
As the UK social care sector navigates a period of profound change, it is important to have people you trust. At Nourish we are building for the future alongside our users, coproducing relevant, effective technology throughout. We are guided by experienced insight, not guesswork. When we work together, and measure what matters, we can build the right systems together, with the right people, to provide the best care all the way down the line.
Want to find out more about a structured and objective approach to assessing people’s evolving needs? Ensuring that care and support plans remain aligned with real-world requirements? Read more about Nourish Transparency, our new product innovation, coming soon.
Life happens in moments. What seems small can be significant, what seems substantial can become an afterthought. Whatever form these moments take, in health, care and support services, they speak to the reality of the experience for the person utilising the service. These moments, or as they are more commonly known ‘incidents’ and ‘accidents’ can be incredibly illustrative. Our ability to understand, record and review these ‘incidents’ has a direct impact on the quality of life for the people supported, the people supporting, and everyone else involved in the service. It is from this baseline of understanding that we can begin to build our responses. By learning from previous experiences to establish proactive and preventative processes.
In health and social care, an incident refers to any unintended or unexpected event that could have or did lead to harm for one or more individuals receiving care or support, team members, or the organisation itself. Which is quite a broad definition! This includes both clinical and non-clinical events. Ranging from medication errors, falls or behavioural events, to breaches of confidentiality or equipment failures.
The impact of incidents can be profound. Physically, individuals may suffer injury, deterioration in health, or delayed recovery. Mentally, the impact can reach even further. Health and care are intrinsically human experiences from every perspective. Anyone involved in the incident may experience anxiety, loss of trust, or trauma. Research by NHS England highlights that unresolved incidents can lead to long-term psychological effects such as post-traumatic stress disorder (PTSD) in both patients and healthcare professionals.
Effective incident management is therefore essential. Prompt reporting, thorough investigation, and transparent communication are key to safeguarding individuals and maintaining public confidence. The NHS Patient Safety Incident Response Framework (PSIRF) emphasises learning from incidents to prevent recurrence and improve care quality.
Information is at the heart of preventative care and support. Information attained by care and support workers every day. The proper recording, reviewing and response to incidents can be transformational for service quality and outcomes.
Quality incident management is a benefit in all care and support settings. However, there are a range of challenges facing providers on this front as well. In the moment of an incident, the natural priority falls on addressing it, rather than recording it. For example, take a fall. You want to immediately support the person who fell. So you can begin recording the information about the fall and the person’s condition, rather than what caused it. This is one of the key reasons why underreporting of incidents remains a challenge for providers.
Some of this information is highly person as well. Which means you need to record it as confidential. Something that is not always a fluid criteria to apply and switch between when using paper, or standalone systems.
In fact, standalone systems can also counterintuitively replicate the issues of disconnection that exist with paper-based systems. When the information is siloed, as in a standalone system, it can be difficult to connect it back to the support you are providing. Which makes the vital incident management you are doing ineffective for driving improved outcomes for the people being supported.
Ultimately, this can reduce the purpose of incident management amongst your team. When people can’t see the benefits of their actions or understand the ‘why?’ of their efforts, enthusiasm drops. With so much to do already, the value of incident management becomes lost in the shuffle of siloed information.
At Nourish we’ve been working closely with our customers to develop a new Incident Management solution. One which puts the person supported at the heart of the process. Offering an efficient, easy to use solution for event logging at the point of care and beyond, to escalation and management. Creating a clear throughline of events that is easy to develop, manage and learn from. We spoke to Anna Goscombe, Director of Quality & Therapeutic Services at IBC Healthcare, about their experience helping us to develop this new product.
“For a whole host of reasons, [our] incident detail wasn’t good enough. Or sometimes it was delayed because information was siloed on different platforms. This all meant you couldn’t rely completely on the accuracy of the data. Or you couldn’t respond quick enough. So again, for all those reasons Nourish improves the quality of service that we’re providing to the person we support because we’ve got a better handle and a better management of incidents. We can better map the trends.
“What I mean when I say map trends, is that we can really understand the full picture. For example, ‘what might be the triggers here for this person?’ or ‘Is it specifically happening in the home? Is it specifically in the community where most incidents are occurring?’
“For example, you can see how many restrictive physical interventions there have been. You can check important factors like if any restraints were used. We can then review previous data and see there were three restraints this month. But there was none for the last two months. Clearly something’s happened.”
This level of detail unlocks whole new worlds of insight for you to share across your service and community.
Prevention is born of proactivity, and effective proactivity is beholden to accurate information. With quality incident reporting IBC are able to better understand the needs of their community. The specific point on restraints can be folded into the wider comprehension of that person’s experience. Their diet, their interests, their sleep pattern, all vital updates of experience that help your team notice trends.
These trends hold the key to providing preventative, quality care and support. As Anna explained to us.
“It is crucial we can notice those things and be able to record triggers like that when providing LD and mental health services. It’s important to do it, but also important to do it in a in a timely manner. Local authorities, placing authorities, commissioners, they all expect it. They expect us to analyse that sort of data, but also to foresee any potential risk or escalation in incidents.
“More than that, we expect it of ourselves. Understanding incidents, even something as basic as that can potentially prevent a hospital readmission, or discharge to another service or staff burnout.”
Keeping teams and communities together can be incredibly challenging in modern care and support environments. Quality incident management can help you meet this challenge. Of course, as always, the success will be determined by the people involved.
It should be obvious by now how important your team members are to this process. They will be the ones at the coalface of this process. It is vital that your care and support teams play an active role in incident management and reporting. One where they can see directly the benefits of their effort and take pride in the positive outcomes they deliver. This cannot be achieved without a positive, reinforcing learning culture.
The PSIRF advises a move away from blame and towards understanding the root causes of incidents. Whether they stem from human error, systemic issues, or gaps in training. The focus on addressing the issue, rather than punishing the cause. With a collaborative and an intuitive, user-friendly system you can engage your team and engender their sense of pride. This adds a tangible personal impact to the weight of their daily workload. Naturally, effective incident management takes time and practise to establish. It’s important to appreciate that everyone has an influential part to play to get it right.
‘Incidents’ and ‘accidents’ are broad terms for a wealth of specific events. Each one of these events, from the small to the substantial, help you better understand your service, and the community it supports. The accuracy and availability of this information trickles through to every other area. Showering the relevant parties with the information they need. Whether they’re at the point of delivery or in the back office. A single stumble can reflect a worsening trend. A quiet smile can reveal a forgotten passion. Every slip can inform your next step, and every step forward will empower your community.
Learn more about how Nourish can help you make the most of every ‘incident’ you have with our upcoming incident management system; Nourish Safety, there isn’t a moment to lose.
Our Concorde Customer Conference was a celebration of everything we’ve been building together with our users, highlighting the teamwork, understanding and innovation that drives us forward
The energy of the day was incredible, as we shared our upcoming roadmap, engaged with innovators from across a range of care and support communities and explored how we can coproduce the best technology, and the best results for providers and the communities they support
Enjoy our short recap video, which highlights the purpose, partnership, and progress we’re making alongside our users here at Nourish
We’re so grateful to everyone who joined us on the day, for their energy, insight and understanding, with 10 amazing years to build upon, and so much planned for the future, there’s never been a better time to come fly with Nourish.



Several of our friends from the Nourish Partnership Programme (NPP) joined us on the day. We integrate with these suppliers. So we can further support a more connected and collaborative care sector. Thank you so much to the partners who joined us on the day. If you’d like to learn more about the NPP click here.
Famileo, Blaucomm Care, Ally Cares, PainChek, Sona, Relish, GHM Communications, Vayyar Care, Camascope, MOA Benchmarking, Workforce, Adaptive Care
We recently attended Scottish Care’s Care at Home & Housing Support Conference 2025
The theme ‘Compassion in Crisis’ highlighted the reality of care at home in Scotland today, the opportunities that lie ahead of us and how we can work together to achieve them
The day featured insightful talks, engaging seminars and an intimate opportunity to connect with people from across home care in Scotland
A crucial aspect of several of the conversations in Glasgow addressed the need to view care for what it truly is, a valuable investment that drives economic growth and community wellbeing at a local and national level
Scottish Care’s Chief Executive, Donald Macaskill
Dr Macaskill discusses the focus of the event. He also details the incredible potential of home care. Explaining how care can be good for both society, and the budget.
Scottish Minister for Social Care and Mental Wellbeing, Maree Todd (SNP)
Minister Todd speaks passionately about home care. She draws upon her personal experience in health and care to understand the needs of the sector. Her insight informs her calls to change the perspective of social care from a ‘cost’ to ‘investment’.
Scottish Care’s Technology and Digital Innovation Lead, Nicola Cooper
Explains the importance of responsible AI. And why keeping a ‘human in the loop’ is so important when building AI models.
You can watch other recap videos and read more about Nourish here.
Technology initiated a sea change in social care. The rapid uptake of digital systems in social care saw the number of providers using digital social care records (DSCRs) double in the past four years. This impacts every aspect of the care community, from the processes we use each day, to the outcomes people using support experience. The benefits a provider can enjoy from ‘going digital’ are well documented. What is less well documented is the impact technology, and by recent extension AI, have on our perspective. Specifically, our perspective of ‘what good looks like’ in social care.
We sat down with Lewis Sheldrake, an expert with over 15 year’s experience working in local government and a legacy of innovative implementations of technology and training to discuss this topic. Lewis won the prestigious Local Government Challenge in 2023 with his novel AI Labs project. This project centred on ‘leveraging AI into all aspects of local government service delivery’. Crucially, in a way that supported emotional intelligence and promoted human interaction, two core tenants that ran through our conversation. We chatted about the changing perspectives on what good looks like in social care; moving from reactivity to proactivity, the relationship between data, AI and benchmarking in care and why we need to be open to new opportunities in technology.
Lewis Sheldrake spoke to us in a personal capacity and not on behalf of any local government or association.



“From a local authority point of view the absolute baseline of what good looks like in social care is not having any kind of substantial safeguarding risks. Not being in a position where you’re leaving your most vulnerable without care. Or not essentially fulfilling some of the statutory duties that are placed upon local authorities under the Care Act.
“You can probably already pick up the fact that a lot of what I’m talking about is the absence of certain things happening, as opposed to it being a positive. I think that, unfortunately, is part of the challenge that we face. Looking at this through the lens of local authorities, it’s mainly focussed on avoiding crises, rather than proactive, aspirational care.
“Whereas if you were to put it from the perspective of a person receiving care, it’s different. For them, it’s having that assurance that the care that they are receiving is safe and of a good quality. So they can live safely and independently in their own home for as long as possible
“This contrast in perspective is critical, and it’s exactly the point from which we must evolve. It creates the space for technology to bridge the gap and, crucially, help redefine what ‘good’ can and should look like in modern social care.”



“Firstly, I think it’s important to understand that by the time someone gets to their local authority they are at a certain level of need. Their needs are relatively acute and consequently are going to require a level of intervention. One that’s likely expensive at that stage. This is the reactive model we’ve become accustomed to.
“We often hear cases where a family member can no longer cope. They’ve been providing informal care to that loved one and they’re burned out. Under the Care Act 2014, the local authority has a statutory duty to assess those needs – and where they meet eligibility criteria, arrange appropriate support. By this stage, the intervention is often urgent, complex, and resource-intensive.
“This is happening at a time where councils are absolutely creaking with the volume and complexity of demand that is arriving at their front door. And I think invariably that so many of these cases could have been foreseen with the right technology and data in place.”



“Absolutely, with the right technology we could intervene earlier to help the person avoid requiring a care package for longer. Keeping them there, living well and independently for longer. Supporting their next of kin to be able to continue to provide that care but also have some respite for themselves. I think this is where technology really can fit in. There are two key components of this.
“The first is about being smart in our uses of data. There are some really good examples from my experience around using data. Such as a council utilising data from other interactions it had with people to help build greater levels of prediction. Initiatives to understand when somebody is deteriorating to such an extent that a proactive intervention would be valuable.
“I know during COVID a council were able to identify with 95% accuracy which of their residents would likely be on the shielding list. Through the use of data, they’re able to accurately predict those people and proactively support them. I also know of councils who utilised data to develop predictive falls models. Again, this significantly changes the effectiveness of care, as we can proactively reach out to at-risk people and offer them interventions. Interventions which, along with improving quality of life for citizens, save the local authorities money.
“The second part of this is through digital technology devices. For example, in the case of falls, a device that can detect when a person falls and activate an alarm in response to send for support. But beyond responding to incidents, there’s increasing potential to analyse the patterns and behaviours that often precede a fall. This allows us not just to react, but to intervene earlier or mitigate the risk before a fall occurs at all.”



“I think both of these aspects, if used coherently, will alleviate the amount of pressure arriving at the front door of local authorities. Both in volume and also in terms of acuity. Now, by the time someone is coming to you for a care package you already have a more rounded understanding of their circumstances. Who they are, the context they live in, and the support networks around them. . The volume of that home care they need is less than it otherwise might have been thanks to earlier, preventative interventions.
“In effect, it helps smooth the peaks in demand – reducing the levels of complexity and acuity of cases presenting at any one time. Which in turn lowers the cost to the council and the financial burden on the person receiving support.”
“It’s central. Broadly, there are two ways of using data to understand need and provide effective care.
“There’s the strategic, macro use of aggregated data across large population groups. This approach is highly effective at generating predictive models that assess risk and identify patterns. Providing valuable insights for both providers and commissioners. It enables more intelligent, data informed decisions about how services are designed and delivered, ensuring they are suitably tailored to meet the needs of their clients. We’ve seen examples of this approach applied with great success in other high-risk sectors, such as the aviation industry.
“The second way, and I think the more exciting side, is the micro, hyper personalised application. Where we can focus down on the individual to really understand their needs and ambitions. Again, we see impressive examples of this data application in other sectors. Such as the preference-driven algorithms behind Amazon, Netflix, and Spotify. As well as personalised customer journeys across digital platforms.
“If you were to think about how some of those principles that underlie their architecture. Albeit very different sectors with very different objectives. It raises an important question: what if that architecture were applied to a health and social care context? How helpful that would be to ensure people are getting exactly what they want and need, when they want and need it?
“One of the most powerful aspects of this shift from reactive to proactive care is the ability to anticipate. In social care, hospitals, and communities, we often hear the same phrases: ‘It was only a matter of time.’ ‘We could see this coming.’ These reflections highlight how predictable many crises are – with hindsight. With the right acquisition and application of data, we can change what good looks like in social care in a positive, person led way.”
“If we break down the core functions that exist in care, there are a number of different actors doing different tasks e.g. care planning, initial assessments, delivery of that care. I think there are really compelling applications for AI for each of those. Applications that can enhance the delivery of that function, while in turn delivering a higher level of quality and precision to the end user.
“We’re already seeing promising examples of AI reducing administrative burden with data entry. In terms of things like transcription and data input. I think it’s a good start, but there is significant untapped potential to expand AI’s role across the wider care ecosystem.
“For any care plan that’s pulled together, you think about how many other care plans have gone before that. Drawing upon the decades of experience and knowledge from the people that are inputting into those care plans. With AI this information can be readily triangulated to make the most precise care plan for any given set of circumstances. AI can prompt follow up actions or suggest referrals based on all the data your service has. These prompts support care decisions rather than automate them. Helping to standardise the service offer based on the individual needs of each client, by drawing upon the wealth of experiences and outcomes across your service to inform best practice. Ideally alleviating the variability of individual social workers, while enhancing the specificity of your care plans.
“The data gathered during this care provision is then fed back into the system. This creates a virtuous cycle of person led, community centred care. And that’s just one quick example. From high level strategy to direct care delivery in people’s homes there are applications for data and AI that improve service quality, operational efficiency and ultimately deliver the objectives that keep people living safely and independently in a place they call home for longer.”
“The most immediate answer is reducing administrative burden. There’s lots of opportunities for AI and care technology in general to afford people more time delivering what they got into the job to do. Face to face care, in a more personalised and informed way.



“Let me offer a counterpoint. There’s a common misconception that, more human care always equates to better care. But in some cases, that’s not true. Overprescription and unnecessarily invasive care can diminish a person’s independence and dignity. Take supported living settings for example. Imagine someone with learning disabilities who receives 24/7 care. There are people coming in, waking them up in the night to routinely check in on them. This is well-intentioned, but disruptive. In such cases, the use of technology there can help provide that person with a more respectful and person-centred alternative. Providing greater levels of privacy, independence and dignity. While still ensuring support is available when genuinely needed.
“My key point is about precision and that is certainly where I think AI can play a transformative role. Ensuring care is sufficiently proportionate to the needs of the individual. I don’t think that necessarily means more care is better. I think it’s about the quality, appropriateness and value of the ‘care’ being provided.
“Care in inverted commas mind you, because we’re using care as a kind of umbrella term for a whole number of things at the moment. A lot of responsibilities that are falling under the umbrella of care are not actual direct care. They are different forms of administrative tasks. We need to think about how to displace that through the use of AI and other digital tools to ensure that we are maximising our resources and delivering the best outcomes possible.”
“Absolutely, I think it has too. We have to be realistic. There are massive capacity challenges both in terms of the workforce, and also in terms of the budgets to support social care.
I personally think there are circumstances where technology could well replace some types of care which are not necessary to be delivered in person. With an ageing population and increasing levels of need and vulnerability, we have to use our finite resources wisely. Care capacity is not limitless, and technology offers a valuable opportunity to redeploy human effort where it’s needed most.”
“Understandably so, there are massive capacity challenges in social care, both in terms of workforce and budget. But rather than viewing these constraints purely as limitations. They invite us to re-examine our definition of ‘good’. They imagine how technology and AI can shape what good looks like in social care into a new vision. One that’s more sustainable, personalised, and outcomes focused.
“So much care provision is historically focussed on things like washing, bathing, food, medication. But if we consider this through the lens of Maslow’s hierarchy of needs. These are foundational; they sit at the base of the pyramid. Essential, yes, but not sufficient for a fulfilling life.”
“What it often fails to address, whether due to technical limitations or lack of resource, is anything related to the higher levels of that hierarchy. Support for self-esteem, companionship, and emotional fulfilment is frequently absent. Let alone opportunities for people to self-actualise!
“I really believe that there’s an opportunity to move away from the primary function of care provision being to give people the bare necessities and to basically keep them alive.
“An opportunity for us to move to a form of care that helps people have a greater level of self-esteem, belonging and purpose. Take social isolation for example. Everyone is aware of our social isolation problem and the significance of its health implications. But actual interventions to address this issue are sparse, largely due to cost.
“I think there is huge potential to augment existing models of care using technology and AI to alleviate some of these kinds of challenges.
“AI tools, even just the currently mainstream ones like ChatGPT offer fascinating potential in supporting social connection, stimulation, and engagement. For some people, these platforms provide opportunities to engage in meaningful conversations they might not otherwise have. Interactions that validate their experiences, challenge their thinking, and stimulate them intellectually. It’s obviously not care in the way that we understand and conceptualise care and certainly traditionally. But when you stop to think about it. If someone is able to enjoy an engaging conversation about a subject that’s meaningful to them, that validates their experience, challenges them and stimulates them intellectually, isn’t that a core tenant of ‘good’ care?
“I think there’s value in that. These possibilities have scope, and the potential to progress much further and I don’t think it should be ruled out. Absolutely, AI and technology can help drive more informed decisions, reduce administrative burden and promote coproduction.
“But if we just look to use technology to fulfil functions already fulfilled by traditional models of care. I think that would be a missed opportunity.”
The future of social care in the UK is linked to the future of the NHS. One cannot progress without the other. So, when the NHS established the Assured Solutions List (ASL) to help shape the future of digital social care, every software supplier in the sector took notice. NHS Assurance is a clear badge of quality and ambition. Nourish Care was the first Digital Social Care Record (DSCR) to join the ASL. A statement of our commitment to both compliance and innovation in care technology.
The purpose of the ASL is to encourage care providers to digitise. By establishing a trusted baseline of system requirements and providing funding to help providers get started. The requirements for membership of the ASL granted confidence to providers of the capabilities of the system they were using to digitise their processes. NHS Assurance guarantees safety, security and reliability for care providers when choosing their digital partner.
Since Nourish joined the ASL, it continues to expand in membership and calibre. This year saw an expansion of standards with the introduction of 14 new standards. These standards built upon the baseline of requirements for assured solutions and indicated the coming ambitions for health and social care interoperability. They covered a range of important issues, including the use of data, information sharing, security and integrations.
It is crucial to use a system that complies with these standards to set yourself up for the future. Most suppliers are still yet to be approved on all 14 standards, you can see how far along they are here. Click on the supplier and navigate to their ‘Standards’ drop down.
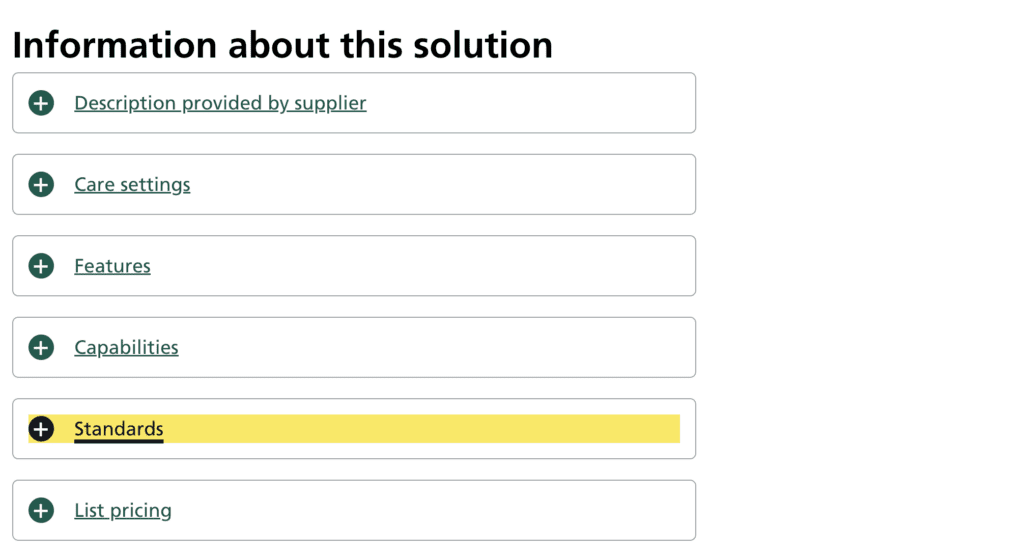
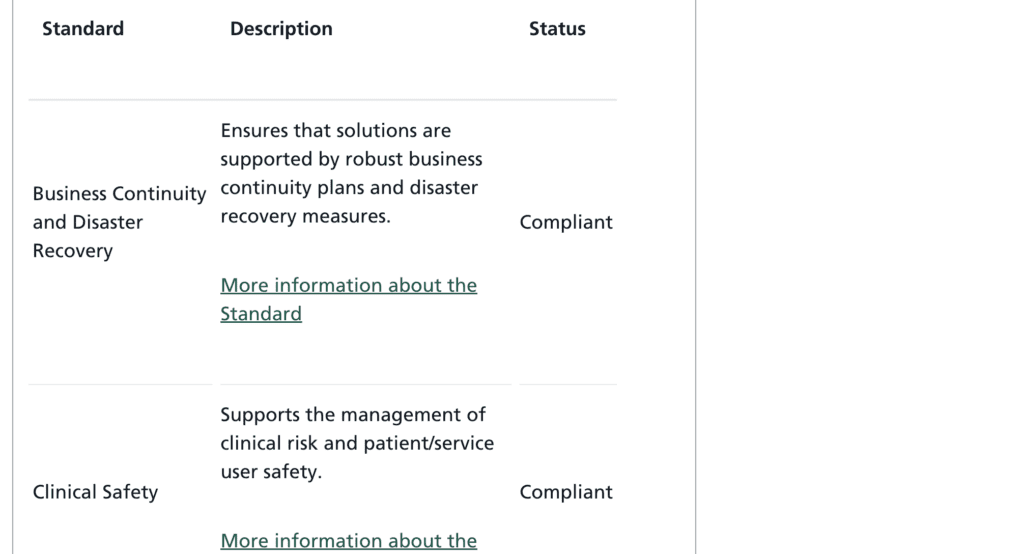
It is clear the NHS have further designs for the ASL and its members. Compliance with the existing standards indicates a supplier is aligned with the future direction of digital social care. When looking to your own future it is important to ask the suppliers you utilise about theirs.
What connections do they have to the NHS?
What is their approach to interoperability?
How committed are they to maintaining their standards of compliance and information security?
Ensuring alignment with your digital supplier is vital for building a future-proof and secure business. Ensuring your system and service are qualified with NHS assurance. If you are curious about switching your digital system to a new supplier, we have prepared a useful document detailing the process with us. You can view it here.
If you would like to learn more about how Nourish works with our users to wrap our system around your service, you can read our case studies here.
One of the clearest requirements of the new 14 standards for NHS Assurance is interoperability. The ability to record, store and share information securely. This is in direct response to the ‘sin of silos’ that plagued health and care providers for decades.
Along with our adherence to these standards Nourish also champions interoperability through the Nourish Partnership Programme. This initiative reflects our commitment to building solutions across suppliers to best serve care providers and their communities. We are proud to develop social care led solutions alongside suppliers, providers and our wider communities.
The NHS and social care move together. In September Wes Streeting announced ‘three key shifts’ for the NHS. With recent developments for the ASL, increased focus on compliance and a commitment to interoperability it is obvious this shift is coming to care as well. We previously explored the move from ‘Analogue to Digital’ here. The ability to deliver the other two key shifts, namely ‘sickness to prevention’ and ‘hospital to community’ will largely be defined by the ability of different health and care providers to share their information with each other. The ‘Data Use and Access Bill‘ highlights this focus from the UK government and points to the significance of membership to the ASL for digital social care records as a baseline.
It is clear digital systems will play a huge role in the future of health and care in the UK. Now is the time to make sure you have a partner you trust, understand and enjoy working with.
Now is the time to talk to Nourish, because things are just getting started.
Compliance is crucial for home care providers. Evidencing compliance is vital for care providers meeting regulations and ensuring compliance is important for providers delivering quality care. Whatever form your regulator takes, or whatever reforms they implement, it is vital you can tell your care story. Home care compliance is particularly important due to the incredibly personal nature of welcoming a carer into your house. It requires a feat of great trust on the part of your customers. A trust that is sacred to the quality of care you provide and the standard of your reputation. Any home care business looking to grow and secure new customers needs to be able to tell their care story effectively. One that shows your compliance with established regulations and ability to support your community.
The right digital partner can help you capture your care stories and share them with all your stakeholders. This can go beyond your regulator, to your wider circles of care and community. All relationships are defined by the trust you share with each party. Nourish Care gives care providers the tools to capture all the information you need, understand it on both a micro and macro level, and build case studies that show the quality of your care.
It is vital you capture the right information to tell your care story from your care delivery. Everyday thousands of small acts of personal empowerment are provided through home care. Don’t sell yourself short by letting them slip through your forms! With the right digital care management system you can rest assured your team is recording everything you need.
Nourish Care records all the information from your team in real time through our app. This simplifies the process of recording, and subsequently reporting, the care you provide. Helping you to tell an accurate care story to your regulator. Home care compliance is further boosted through the audit trail capabilities of our system. This charts all actions on the Nourish platform, giving you a clear timeline of activities. Which in turn ensures care delivered can be easily evaluated to promote quality as well as the right care being delivered to meet people’s needs, wishes and preferences.
This is particularly important for home care providers who need to report actual appointment times. We offer a selection of call monitoring options, including devices and a start/stop button on our app. This guarantees a wealth of information for your coordinator. Information including the actual appointment times and the location of the sign in, as well as capturing all of the relevant interactions that occur during the appointment.
Each of the interactions captured during an appointment constitutes a data point. What they ate, when they ate, what exercises they did, where they went, what they drank, how they felt. Nourish automatically plots these data points for you, weaving a tapestry of information on your care delivery for you to share.
You can use the information Nourish presents you with to identify trends. Trends that unlock a deeper understanding of your care for everyone involved with your service. Your coordinators will be able to comprehend the nature of your care on a range of levels. This provides valuable oversight whether you are a small family-run business or operating as a franchise!
Crucially, it makes it simpler for you to be able to chart and detail your care for your inspector. Show how you engage, understand and respond to the needs of your community over time. A comprehensive, and comprehensible, overview of your service sets the scene perfectly for the nature of your care. Allowing you to then guide your inspector through specific examples and case studies to acquaint them with the day-to-day reality of your care.
Case studies are one of the clearest ways to inform people about your approach to care. We have several of them ourselves we’d love you to check out!
Care is not a static undertaking. Living the life you want is about having the freedom to pursue your interests. Quality home care supports people to do just that. Quality home care software supports providers to record, review and report their life-changing care.
Nourish gives you the tools to build case studies of the people utilising your service. These case studies detail on a one-to-one level of how you wrap your service around your clients. Demonstrate the unique way you provide care to your community, illustrating how you involve people with support and their circles of care. Document appointments and demonstrate how you respond to your client’s needs as they evolve and develop thanks to your support.
Our robust home care app makes involving people in their care decisions simple. Voice-to-text technology and note-taking capabilities means your carers can engage directly with your client’s experiences and record them in Nourish. Showing the person-led approach to care that is championed by regulators across the UK and Ireland.
Home care compliance is more than a box-ticking exercise. It is an opportunity for you to share the incredible care you provide. Too often the true depth of care goes unacknowledged during an inspection. With the right digital home care software you can ensure that every aspect of your outstanding approach is captured.
Regulations will continue to grow and adapt with time, just as will your service and the communities you support. That’s why it is vital you can tell your care story, utilising home care software you trust.